Nerve Stimulation To Treat Urinary Incontinence
Many people have heard of pacemakers and how they can be used to treat heart conditions. But did you know a similar implantable device is available to treat urinary incontinence?
Urinary incontinence, or the loss of bladder control, is common. One of the most common types is urge incontinence, which is distinguished by a sudden, intense urge to urinate followed by an involuntary loss of urine. About 17% of women and 3%11% of men experience urge incontinence at some point in their lives.
Symptoms of incontinence can cause people to feel socially isolated, experience sexual inhibition, or become afraid to make social or travel plans. Careers and personal relationships are often affected.
Fortunately, many treatment options can help, including sacral neuromodulation.
What Are The Benefits And Potential Side Effects Or Complications Of Medtronic Bladder Control Therapy
Medtronic Bladder Control Therapy may reduce symptoms for many people who suffer from urinary retention. It can also significantly improve quality of life. Medtronic Bladder Control Therapy is reversible and can be discontinued at any time by turning off or removing the device. Unlike other surgical treatment options for urinary retention, Medtronic Bladder Control Therapy starts with an evaluation. During this evaluation you can experience how it feels and how it works, prior to going forward with the implant procedure.
Implanting the InterStim System has risks similar to any surgical procedure, including swelling, bruising, bleeding, and infection. Talk with your doctor about ways to minimise these risks.
Medtronic Bladder Control Therapy might cause you to experience some of these side effects:
- Pain at the implant site or new pain
- Infection or skin irritation
- Interactions with certain other devices or diagnostic equipment
- Undesirable changes in urinary or bowel function
- Uncomfortable stimulation
Problems may be resolved with surgery, medication, or programming. These events may also resolve over time. There is a possibility that some may remain unresolved. See Important Safety Information for possible adverse events. Please consult your doctor. This therapy is not for everyone. A prescription is required.
Pelvic Floor Muscle Exercises
Pelvic floor muscle exercises, also known as Kegels, can help improve incontinence and prevent it from worsening. They can help you suppress the urge to urinate. The exercises strengthen and tone the muscles that support the pelvic organs. These muscles contract and relax under your command to control the opening and closing of the bladder. When these muscles are weak, urine leakage may occur. To achieve the best results, imagine yourself as an athlete in training. You need to build strength AND endurance of your muscles. This requires commitment and regular exercise. Correct technique also is very important.
For more information on how to perform Kegels, see our Patient Information page.
Don’t Miss: Causes Of Repeated Bladder Infections
Other Sites Of Electrical Stimulation
One of the first techniques for the treatment of lower urinary tract storage dysfunction stimulated the suprapubic region in patients with painful bladder syndrome , . This method was used to relieve abdominal pain, similarly to the principle of TENS when used for the relief of pain presumably. Subsequently these patients also experienced reduced urinary frequency . Two later studies documented an improvement in urodynamic parameters in patients with detrusor overactivity , sensory urgency, or neurogenic problems. However, based on the literature, the efficacy of stimulation of a suprapubic site in patients with OAB symptoms is unproven , .
Another reported approach has used stimulation of the thigh muscle in spinal cord injury patients to relieve spasticity. In some of these cases, this has led to improvements of urgency incontinence as well as an increase in the maximum cystometry capacity and reduced maximum detrusor pressure , . Further to this 6/19 patients reported clinical improvement in urinary incontinence and frequency extending out to 3 months after treatment .
Based on this, at best limited evidence for stimulation at other sites, the most logical approach to be used in transcutaneous electrical stimulation techniques appears to be either sacral stimulation or PTNS as they either directly or indirectly target the S3 spinal cord root.
How Effective Is Interstim Therapy

The InterStim® System, is an effective, long-term treatment that is clinically proven to:
- Significantly improve quality of life
- Relieve symptoms when other treatments fail
- InterStim® Therapy is clinically proven to improve bladder control in people who have not had success with other treatments, such as oral medication, behavioral therapies, and dietary and fluid changes.
In a long -term clinical study, it was found that 59% of patients with urge incontinence who received the InterStim® System and completed follow-up with their doctors had at least 50% fewer leaks per day when compared to the number of leaks before therapy.
Read Also: Does Alcohol Cause Bladder Infections
Clinical Applications Of Electrical Stimulation For Bladder Control
Different locations have been investigated for application of electrical stimulation to restore functional bladder control, each with varying degrees of success. In the past, electrodes for stimulation to modulate bladder function have been placed on the bladder, skin, peripheral nerves, sacral roots, or spinal cord. Fig. depicts the neural innervation of the lower urinary tract and common electrode locations for restoration of bladder control. The effectiveness of recently developed applications of electrical stimulation for bladder control has been evaluated in clinical studies in persons with SCI, although not in randomized, controlled clinical trials. The associated morbidities in patients with SCI adds complexity to the understanding of how each approach might be used to treat NLUTD, and the optimal, or even suitable, therapy is likely to vary across individuals.
There has been limited clinical success with direct bladder wall stimulation due to problems with concomitant sphincter activation caused by reflex activity evoked by activation of pelvic afferents in the bladder, pain, or device failure. Pelvic nerve stimulation, i.e. stimulation of the nerve supply to the bladder, was shown to produce bladder contractions in dogs, but also resulted in co-activation of urethral sphincters. Pelvic nerve stimulation requires lower amplitudes of stimulation than direct bladder wall stimulation but application in humans is limited due to the difficulty of electrode placement.
The Science Behind Sacral Neuromodulation
One way the brain controls our bodys muscles and movements is through electrical messages, which are carried by nerves. These nerves have major routes with smaller pathways running off them.
One major route runs from the brain, along the spinal cord and through the lower back called the sacral area. Here, nerve paths split off and go in different directions, some to the pelvic area. The muscles in the pelvic area, such as the pelvic floor, urethral sphincters, bladder and anal sphincter muscles are controlled by the brain through nerves that run from the sacral area. Our sensations, such as fullness in the bladder or rectum, are also relayed to the brain via these nerve routes.
Sacral Neuromodulation helps to correct inappropriate, unwanted or even erroneous messages sent along these nerve pathways.
You May Like: Treating Overactive Bladder In The Elderly
Bladder Dysfunction After Sci
Neurological disease and injury can cause significant disruption of both the storage and emptying functions of the LUT. SCI, specifically, causes LUT dysfunction characterized by neurogenic detrusor overactivity, urinary incontinence, chronic urinary retention , and DSD. The location and severity of the SCI affect the degree of bladder dysfunction, from interrupting the communication between sacral and pontine micturition centers, to directly damaging the lumbosacral circuits that control the detrusor and pudendal nerve output. Spinal cord injuries are classified on a scale by the American Spinal Injury Association , where A describes complete spinal transection where no sensory or motor function is preserved and E describes normal spinal cord function. Bladder dysfunction leads to substantial decreases in quality of life and can cause urinary tract infections, skin breakdown, bladder and kidney damage, and re-hospitalization., Further, bladder dysfunction caused by SCI may change over the course of the injury, for example changing from an areflexic to an overactive bladder with time following injury, making bladder management difficult.
The goals of management of NLUTD, including NDO, are protection of the upper urinary tract, improvement of urinary incontinence, restoration of LUT function, and improvement in quality of life.
Here Are Answers To Common Questions About This Treatment Option:
How long do you need to have symptoms before seeking treatment?
Talk with your primary care provider or OB-GYN if you have experienced symptoms of urinary incontinence for six months or longer. First and foremost, our approach is to try to understand what is contributing to your symptoms.
Do you need to try other treatment options first?
Yes, you’ll usually try other treatment options first. Three categories of treatments are available for urinary incontinence, and the most appropriate option will depend on the cause of your symptoms.
First-line treatments include conservative treatments, such as making lifestyle changes to train your bladder or physical therapy, including pelvic floor and Kegel exercises. Second-line treatments include medication therapy. The first medication was approved by the FDA in 2003 and many options became available since that time. Each person responds differently to medication therapy, so it’s good to have options.
The first two categories of treatment provide symptom relief for about 75% of people. By the time we are discussing a sacral neuromodulation procedure, you’ll have tried and failed treatment options from the first two categories or couldn’t tolerate the side effects.
How does sacral neuromodulation work?
With sacral neuromodulation, a small device is inserted under your skin in your lower back. Small wires, called leads, send low-level, mild electrical impulses to your sacral nerves.
Can I try sacral neuromodulation before committing?
Recommended Reading: What Is The Treatment For Low Grade Bladder Cancer
Biofeedback And Electrical Stimulation: 2 Complementary Techniques
Electrical stimulation can be used before using biofeedback. This technique can be useful if you dont feel if you contracted your pelvic floor muscles or if you dont know how to contract it.
Varying the intensity of the electric current makes it possible to workout your pelvic floor muscles in different ways. According to the chosen program, you can work on different types of incontinence.
Once you feel your pelvic floor enough to contract it by yourself, you can change and train with biofeedback.
If you already know how to contract it, you can use biofeedback right away.
More interesting information about the pelvic floor and helpful exercices you can find in our free app:
Are Acute Effects Of Stimulation Of Clinical Significance
An obvious approach to answer this question would be to assess the effectiveness of electrical stimulation in suppressing detrusor overactivity , chosen because it presents in many patients with OAB symptoms . This has led researchers to investigate the acute effects of electrical stimulation during an urodynamic study.
Similarly inconsistent effects apply for acute TPTNS studies, although Amarenco et al. reported positive results in half of the neurogenic disease patients he studied. These patients showed a 50% improvement in volume at the first detrusor contraction and/or MCC of more than 50% of the baseline value. A previous urodynamic study showed no significant differences in any of the urodynamic parameters in 36 detrusor overactivity patients . This differing result might arguably be due to different pathologies seen in the patients.
Neither of the two approaches to the investigation of acute effects, at either stimulating site, has clearly and robustly demonstrated effectiveness. Nevertheless, the balance of the literature indicates that patients may benefit from neuromodulation effects which may arise from repeated stimulation sessions rather than a single application. In addition, de Seze et al. concluded that treatment may be effective even in patients who did not respond to an initial acute TTNS applied during urodynamic testing.
Don’t Miss: What Happens With Bladder Cancer
Pudendal Nerve Stimulation In Sci As An Alternative To Sacral Nerve Stimulation
Peripheral nerve stimulation is an alternative approach to target similar reflexes as sacral nerve stimulation, potentially with more specificity. In contrast to PNS, which targets a particular nerve or nerve branch, SNS with Interstim® targets the entire sacral nerve. The use of this non-selective location results in non-specific stimulation of both afferent and efferent fibers. This ambiguity contributes to the lack of understanding of the mechanisms by which sacral nerve stimulation works and why it remains ineffective for treatment of NLUTD after complete SCI. Because SNS is effective for the treatment of non-neurogenic bladder dysfunction and less successful for patients with complete SCI, there is speculation that preserved supraspinal connections are necessary for the positive effects of SNS. Many studies have identified that the primary effects of PNS occur through activation of spinal reflexes,, which remain intact following supra-sacral SCI. This mechanistic difference is further corroborated by studies where patients with SCI experienced better symptom improvement with PNS than SNS.
What Is Interstim Therapy And How Does It Work
InterStim® Therapy is a proven neuromodulation therapy that targets the communication problem between the brain and nerves that control the bladder. If those nerves are not communicating correctly, the bladder will not function properly.
The InterStim® system uses an external device during a trial assessment period and an internal device for long-term therapy. You and your doctor may decide to try InterStim® Therapy by going through a trial assessment, you and your doctor will determine the next step that is right for you.
Recommended Reading: How To Find Out If You Have Bladder Cancer
When Your Bladder Or Bowels Control Your Life
Everybody has to go. For those of us with neurological conditions like spinal cord injury, multiple sclerosis, or even complications from a stroke, you can often feel tethered to the toilet. In fact, bladder and bowel control consistently rank among the most important functions to regain among people living with spinal cord injury, according to a study led by Dr. Kim Anderson-Erisman of the Miami Project that surveyed nearly 700 cohorts.
Understanding bladder and bowel options starts with knowing how the systems work. The urinary system consists of an upper tract and a lower tract. The upper tract includes the kidneys and ureters the ducts that drain urine from the kidneys. The lower tract consists of the bladder, sphincter and urethra. Think of the bladder as the bodys holding tank for urine, while the sphincter is the door and the urethra is the pathway. In a normal functioning system, when the bladder is full, a sensory signal sent to the brain says, Hey, you need to go. Once you are in an appropriate position to release, a signal is sent from the brain through the spinal cord telling the sphincter to relax and open the door, allowing urine to pass through the urethra. But for those of us with neurological conditions, the process doesnt work like that.
What Can I Expect In The Typical Pre
Typically, an in-office test is done called a peripheral nerve evaluation essayswriting.org. The diagnostic evaluation is a minimally invasive procedure with no incision. The average evaluation lasts from 15-30 minutes. Your physician will begin by numbing your skin with local anesthetic and then placing two small thin wires under the skin near the tail bone with a needle. The nerves that control bladder function are found below this area.
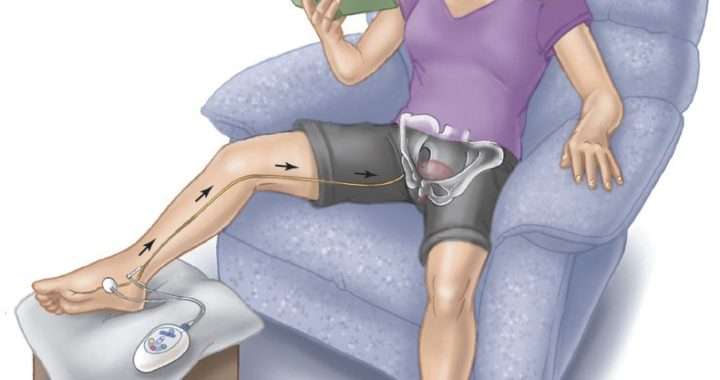
The two thin wires will be attached to an external device which will accompany you for approximately three to five days. The device will provide mild pulses of energy to the nerves that control the bladder as you return to your normal activities. Over the course of the test period, if you show an improvement in symptoms of 50% or greater, you may be a candidate for long-term treatment with Axonics or InterStim therapy.
The long-term implant is a minimally invasive procedure that is usually performed under local anesthesia on an outpatient basis. The surgical implantation typically takes no longer than 45 minutes to perform.
The incision area may feel sore and/or painful for a couple of weeks. This will lessen as you heal. You may return to your doctors office a few more times over a 6-month period to fine-tune your stimulation settings. Once adjusted to achieve the best control of your symptoms with the least discomfort, you may need to return to your physicians office for check-ups only once or twice a year.
Also Check: Bladder Cancer Recurrence After 5 Years
On The Research Front
With all these options, there is still much activity on the research front to find better solutions, particularly in the medical device realm. The Craig H. Neilsen Foundation has put efforts toward further research, and the National Institutes of Health specifically identified bladder and bowel control as a key area for development in their five-year research plan. So, what is actually happening on this front? A list of human clinical trials can be found through clinicaltrials.gov, but here are a few highlights:
A company called Spinal Singularity is developing the Connected Catheter. Led by Derek Herrera, who lives with paraplegia, the company is working on a device that is an extended use, internally inserted, smart catheter. It has a pressure sensor to notify the user when the bladder is full and needs to be drained. The device has a valve to open and close the urethra upon command by the user. It is designed to minimize unexpected leakage and the need for an external leg bag. It is currently under development with clinical trials in the United States projected later in 2017.
The ultimate goal of research is to improve quality of life for people with SCI or other neurological disorders. If our approaches are successful, we hope to improve confidence, independence, and dignity for these individuals as well as significantly reduce costs and burdens related to care, says Bourbeau.
What Is Functional Electrical Stimulation
Functional electrical stimulation applies small electrical pulses to paralyzed muscles to restore or improve their function.
FES is commonly used for exercise, but also to assist with breathing, grasping, transferring, standing and walking. It can also lead to improved bladder and bowel function. There’s even evidence that FES may reduce the frequency of pressure sores and urinary tract infections.
The excitement around FES technology really sparked in 1983 when Nan Davis, a paraplegic student at Wright State University, got out of her wheelchair and “walked” to get her diploma. She was powered by an FES system and inspired a TV movie called “First Steps.”
The Wright State technology soon emerged commercially in the form of a stationary bicycle called the Regys in which users pedal the bike using FES-stimulated leg muscles. Researchers soon noted that this form of FES provides real aerobic exercise in people who otherwise can’t move on their own, boosting heart and lung function, improving strength and circulation, building muscle mass, even in people with high quadriplegia.
There are some risks associated with FES. Fracture of leg bones is possible due to loss of bone mineral density. Also, FES can trigger autonomic dysreflexia in upper-level injuries. People with severe spasticity, contractures, or osteoporosis are not good candidates.
Read Also: How Can I Heal My Bladder Naturally