Morphologic Variants Of Urothelial Carcinoma
Some cases of urothelial carcinoma show morphologic patterns that are recognized as variants morphology. Those include nested variant, micropapillary, lymphoepithelioma-like, sarcomatoid, small cell carcinoma, and adenocarcinoma. These are frequently under-recognized in bladder biopsies and could have therapeutic implications with different criteria for surgery and different chemotherapy regimens.
Low Grade And High Grade
Bladder cancer can also be described as either low grade or high grade.
Low grade bladder cancer means that your cancer is less likely to grow, spread and come back after treatment. High grade means your cancer is more likely to grow spread and come back after treatment.
For example, if you have early bladder cancer but the cells are high grade, youâre more likely to need further treatment after surgery. This is to reduce the risk of your cancer coming back.
Low grade is the same as grade 1. High grade is the same as grade 3. Grade 2 can be split into either low or high grade. Carcinoma in situ tumours are high grade.
You May Like: How Deadly Is Squamous Cell Carcinoma
Invasion Into The Lamina Propria
Urinary Bladder Tumour, Transurethral Resection: - INVASIVE HIGH-GRADE PAPILLARY UROTHELIAL CARCINOMA with lamina propria invasion.-- Muscularis propria present, NEGATIVE for muscularis propria invasion.-- NEGATIVE for lymphovascular invasion.-- Please see synoptic report.
Block letters
URINARY BLADDER LESION , TRANSURETHRAL RESECTION URINARY BLADDER TUMOUR : - INVASIVE HIGH-GRADE PAPILLARY UROTHELIAL CARCINOMA WITH LAMINA PROPRIA INVASION.- MUSCULARIS PROPRIA NEGATIVE FOR INVASIVE MALIGNANCY.- NEGATIVE FOR LYMPHOVASCULAR INVASION.
Recommended Reading: What Is Stage 4 Melanoma Cancer
Recommended Reading: What Does The Start Of A Bladder Infection Feel Like
Risk Groups For Early Bladder Cancer
Doctors classify bladder cancer that has not grown into the muscle layer of the bladder wall into risk groups. These risk groups are based on several factors, including the size and grade of the cancer. The risk groups allow the doctor to estimate the chance that the cancer will come back and continue to grow and spread . Doctors also use the risk groups to help plan the best treatment.
Any non-invasive and non-muscle-invasive bladder cancers are classified as low, intermediate or high risk.
Papillary Vs Flat Cancer
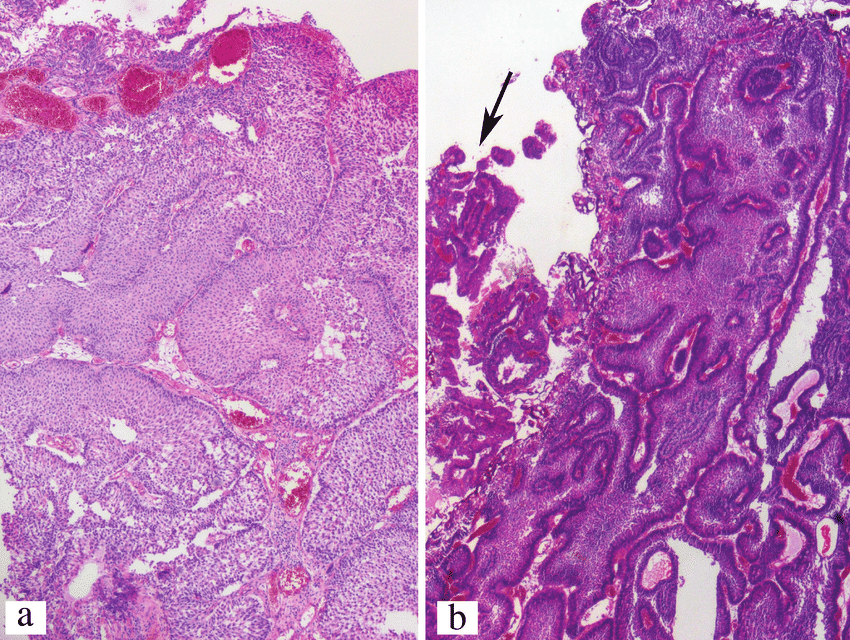
Bladder cancers are also divided into 2 subtypes, papillary and flat, based on how they grow .
- Papillary carcinomas grow in slender, finger-like projections from the inner surface of the bladder toward the hollow center. Papillary tumors often grow toward the center of the bladder without growing into the deeper bladder layers. These tumors are called non-invasive papillary cancers. Very low-grade , non-invasive papillary cancer is sometimes called papillary urothelial neoplasm of low-malignant potential and tends to have a very good outcome.
- Flat carcinomas do not grow toward the hollow part of the bladder at all. If a flat tumor is only in the inner layer of bladder cells, it’s known as a non-invasive flat carcinoma or a flat carcinoma in situ .
If either a papillary or flat tumor grows into deeper layers of the bladder, it’s called an invasive urothelial carcinoma.
Don’t Miss: How Do Doctors Test For Bladder Infection
Treating Bladder Cancer That Progresses Or Recurs
If cancer continues to grow during treatment or comes back after treatment , treatment options will depend on where and how much the cancer has spread, what treatments have already been used, and the patient’s overall health and desire for more treatment. Its important to understand the goal of any further treatment if its to try to cure the cancer, to slow its growth, or to help relieve symptoms as well as the likely benefits and risks.
For instance, non-invasive bladder cancer often comes back in the bladder. The new cancer may be found either in the same place as the original cancer or in other parts of the bladder. These tumors are often treated the same way as the first tumor. But if the cancer keeps coming back, a cystectomy may be needed. For some non-invasive tumors that keep growing even with BCG treatment, and where a cystectomy is not an option, immunotherapy with pembrolizumab might be recommended.
Cancers that recur in distant parts of the body can be harder to remove with surgery, so other treatments, such as chemotherapy, immunotherapy, targeted therapy, or radiation therapy, might be needed. For more on dealing with a recurrence, see Understanding Recurrence.
Other Terms Often Used To Describe Bladder Cancer
Although bladder cancer types are assigned based on the cells that the cancer originates from, several other terms may be used to describe the disease.
- Advanced bladder cancer is another term that may be used to describe metastatic bladder cancer. It means that the cancer has spread to distant parts of the body such as the lungs, bones, liver, or lymph nodes outside the pelvis.
- Locally advanced bladder cancer refers to cancer that has grown through the bladder wall, and possibly into nearby lymph nodes or organs, but has not spread to distant sites in the body.
- Bladder cancer stage describes where the cancer is located within the bladder and any sites of spread. As described above, the TNM staging system assigns a patients bladder cancer to a tumor , lymph node and metastasis category. These categories may also be combined to give an overall stage number: an overall stage of 0 or 1 describes early disease, while stage 4 is the most advanced. For further information regarding staging, see Bladder Cancer Stages.
- Bladder cancer grade is based on the microscopic appearance of cancer cells and suggests how fast a cancer might grow. Low-grade cancer cells appear similar to normal cells and usually grow slowly, whereas high-grade cancer cells have a very abnormal appearance and tend to grow quickly. High-grade cancers are more likely than low-grade cancers to spread.
Also Check: Can Soda Cause Bladder Infection
Cancerous Tumours Of The Bladder
A cancerous tumour of the bladder can grow into nearby tissue and destroy it. It can also spread to other parts of the body. Cancerous tumours are also called malignant tumours.
Bladder cancer is often divided into 3 groups based on how much it has grown into the bladder wall.
- Non-invasive bladder cancer is only in the inner lining of the bladder .
- Non–muscle-invasive bladder cancer has only grown into the connective tissue layer .
- Muscle-invasive bladder cancer has grown into the muscles deep within the bladder wall and sometimes into the fat that surrounds the bladder.
How Is Bladder Cancer Detected
Several tests and procedures, including non-invasive genomic urine tests like Cxbladder, are available to determine whether an individual has bladder cancer or to establish an alternative diagnosis. Some of these clarify the presence of symptoms and others identify alternative causes of these symptoms . Importantly, these tests and procedures are used in combination to determine an overall diagnosis.
Don’t Miss: Can Hernia Mesh Cause Bladder Problems
Types Of Bladder Cancer
The type of bladder cancer depends on how the tumors cells look under the microscope. The 3 main types of bladder cancer are:
-
Urothelial carcinoma. Urothelial carcinoma accounts for about 90% of all bladder cancers. It also accounts for 10% to 15% of kidney cancers diagnosed in adults. It begins in the urothelial cells found in the urinary tract. Urothelial carcinoma is sometimes also called transitional cell carcinoma or TCC.
-
Squamous cell carcinoma. Squamous cells develop in the bladder lining in response to irritation and inflammation. Over time, these cells may become cancerous. Squamous cell carcinoma accounts for about 4% of all bladder cancers.
-
Adenocarcinoma. This type accounts for about 2% of all bladder cancers and develops from glandular cells.
There are other, less common types of bladder cancer, including sarcoma of the bladder and small cell bladder cancer, among others. Sarcomas of the bladder often begin in the fat or muscle layers of the bladder. Small cell bladder cancer is a rare type of bladder cancer that is likely to spread to other parts of the body.
Relevance Of The International Bcg Shortage To The Aua Guidelines
The global shortages in TICE BCG that occurred in 2014 and 2019 led the AUA to recommend several management strategies to maintain high quality care for patients with NMIBC. These recommendations may supersede the guideline statements below. In particular, the BCG shortage impacts guideline statements 17, 20, and 21. The AUA Statement on the BCG Shortage is available at .
Recommended Reading: Does Alcohol Cause Bladder Infections
Irocker Cruiser Paddle Board
Newbie boarders with a spot of curiosity and magical journey in their spirit. Outfitted with an extra-wide 33 base, broad tail, as well as balance functions making this board the steadiest iSUP on the marketplace. With a 400lbs weight capability, its developed to manage any kind of rider.
Stand up with convenience and also try some on-board yoga sensation secure above water the perfect novice board to feed that daring side. A smooth introduction to paddleboarding that will certainly make you rely on yourself!
What Is The Prognosis For Someone With Prcc
The estimate of how a disease will affect you long-term is called prognosis. Every person is different and prognosis will depend on many factors, such as
- Where the tumor is in your body
- If the cancer has spread to other parts of your body
- How much of the tumor was taken out during surgery
If you want information on your prognosis, it is important to talk to your doctor. NCI also has resources to help you understand cancer prognosis.
Doctors estimate survival rates by how groups of people with PRCC have done in the past. Because there are so few people with PRCC, these rates may not be very accurate. They also cant consider newer treatments being developed.
In general, type 2 papillary renal cell carcinoma has a poorer prognosis than type 1.
Related Resources
Recommended Reading: How Do Doctors Test For Bladder Cancer
Muscle Invasive Urothelial Carcinoma
Muscle invasive urothelial carcinoma tumors have spread into or through the muscle layer of the bladder wall.
- T2 tumors have spread into the muscle layer of the bladder wall.
- T3 tumors have spread through the muscle layer and into the fatty tissue surrounding the bladder.
- T4 tumors have spread to nearby pelvic organs, the pelvic wall, or the abdominal wall.
As well as assigning a T category, the commonly used TNM clinical staging system also assigns urothelial carcinoma to an N category and an M category . For further information regarding bladder cancer classification, see Bladder Cancer Stages.
Bladder Instillation Of Chemotherapy
Instillation of chemotherapy drugs into the bladder can reduce the incidence of superficial cancer recurrences, but no single drug has been confirmed to reduce progression of superficial cancer to invasive bladder cancer. This means that multiple small new cancers can be prevented, but progression to a more invasive bladder cancer may occur despite treatment.
The optimal time to administer chemotherapy is immediately after TUR, as the drugs might prevent reseeding of cancer cells that were disrupted with surgery. Mitomycin is probably the preferred drug because it produces few side effects and is not well absorbed into the system, which allows more of the drug to remain in the bladder to treat the cancer. Thiotepa is rapidly absorbed and produces low blood counts. Doxorubicin produces the most local side effects.
Also Check: New Drug For Overactive Bladder
Bcg Relapse And Salvage Regimens
Guideline Statement 22
22. In an intermediate- or high-risk patient with persistent or recurrent disease or positive cytology following intravesical therapy, a clinician should consider performing prostatic urethral biopsy and an upper tract evaluation prior to administration of additional intravesical therapy.
Discussion
Urothelial carcinoma, particularly CIS, is considered a field-change disease with the entire urothelium at risk in affected individuals. Clinicians should remain aware of sites outside the bladder as potential sources for metachronous tumors. While the initial diagnostic evaluation includes radiographic/endoscopic visualization of the entire urinary tract, the extra-vesical urothelium remains at long-term risk for subsequent tumor development. Moreover, these sites may harbor disease and contribute to cancer recurrence within the bladder.
Of note, the Panel recognizes that evaluation of the upper urinary tract and urethra may be withheld in select patients who have received a single induction course of intravesical BCG and subsequently have persistent evidence of disease and are to undergo a second course of BCG.
Guideline Statement 23
23. In an intermediate- or high-risk patient with persistent or recurrent Ta or CIS disease after a single course of induction intravesical BCG, a clinician should offer a second course of BCG.
Discussion
Guideline Statement 24
Discussion
Guideline Statement 25
Discussion
Guideline Statement 26
Start And Spread Of Bladder Cancer
The wall of the bladder has many several layers. Each layer is made up of different kinds of cells .
Most bladder cancers start in the innermost lining of the bladder, which is called the urothelium or transitional epithelium. As the cancer grows into or through the other layers in the bladder wall, it has a higher stage, becomes more advanced, and can be harder to treat.
Over time, the cancer might grow outside the bladder and into nearby structures. It might spread to nearby lymph nodes, or to other parts of the body.
Read Also: How Can I Relax My Bladder Naturally
Stage I Bladder Cancer
Patients with Stage I bladder cancer have a cancer that invades the subepithelial connective tissue, but does not invade the muscle of the bladder and has not spread to lymph nodes. Stage I disease is classified as a âsuperficialâ bladder cancer.
Standard initial treatment for all patients with Stage I bladder cancer is also a transurethral resection with electrical or laser thermal destruction of all visualized cancer.
Rarely, for more extensive or multiple superficial cancers, a segmental cystectomy is necessary. Even more rarely, radical cystectomy is used for extensive multiple superficial cancers. To learn more about TUR, go toSurgery for Bladder Cancer.
Surgery alone is effective in preventing recurrences in approximately 50% of patients with superficial bladder cancer. Failure of treatment is usually due to the appearance of new superficial cancers, which can be retreated with TUR and cautery or laser therapies. Within 15 or 20 years, more than half of surviving patients will have experienced progressive cancer or, more commonly, will develop new cancers, including cancers of the upper urinary tract . Approximately 20-30% of these cancers will require treatment with a cystectomy.
Treating Stage 0 Bladder Cancer
Stage 0 bladder cancer includes non-invasive papillary carcinoma and flat non-invasive carcinoma . In either case, the cancer is only in the inner lining layer of the bladder. It has not invaded the bladder wall.
This early stage of bladder cancer is most often treated with transurethral resection with fulguration followed by intravesical therapy within 24 hours.
You May Like: Feels Like I Have To Pee But Bladder Is Empty
Urothelial Carcinoma With Trophoblastic Differentiation
More than 30 cases of urothelial carcinoma with areas of trophoblastic differentiation have been reported and a small subset has had symptoms related to excess human chorionic gonadotropin production including gynecomastia., , , , Although some of the early reports have described tumors that apparently were composed solely of tissue resembling choriocarcinoma, most tumors reported in the last three decades or so have been composed of a mixture of urothelial carcinoma with trophoblastic elements. A single case of micropapillary carcinoma with trophoblastic elements has been reported.
Figure 11
Also Check: Can Merkel Cell Carcinoma Be Cured
Prognosis And Life Expectancy
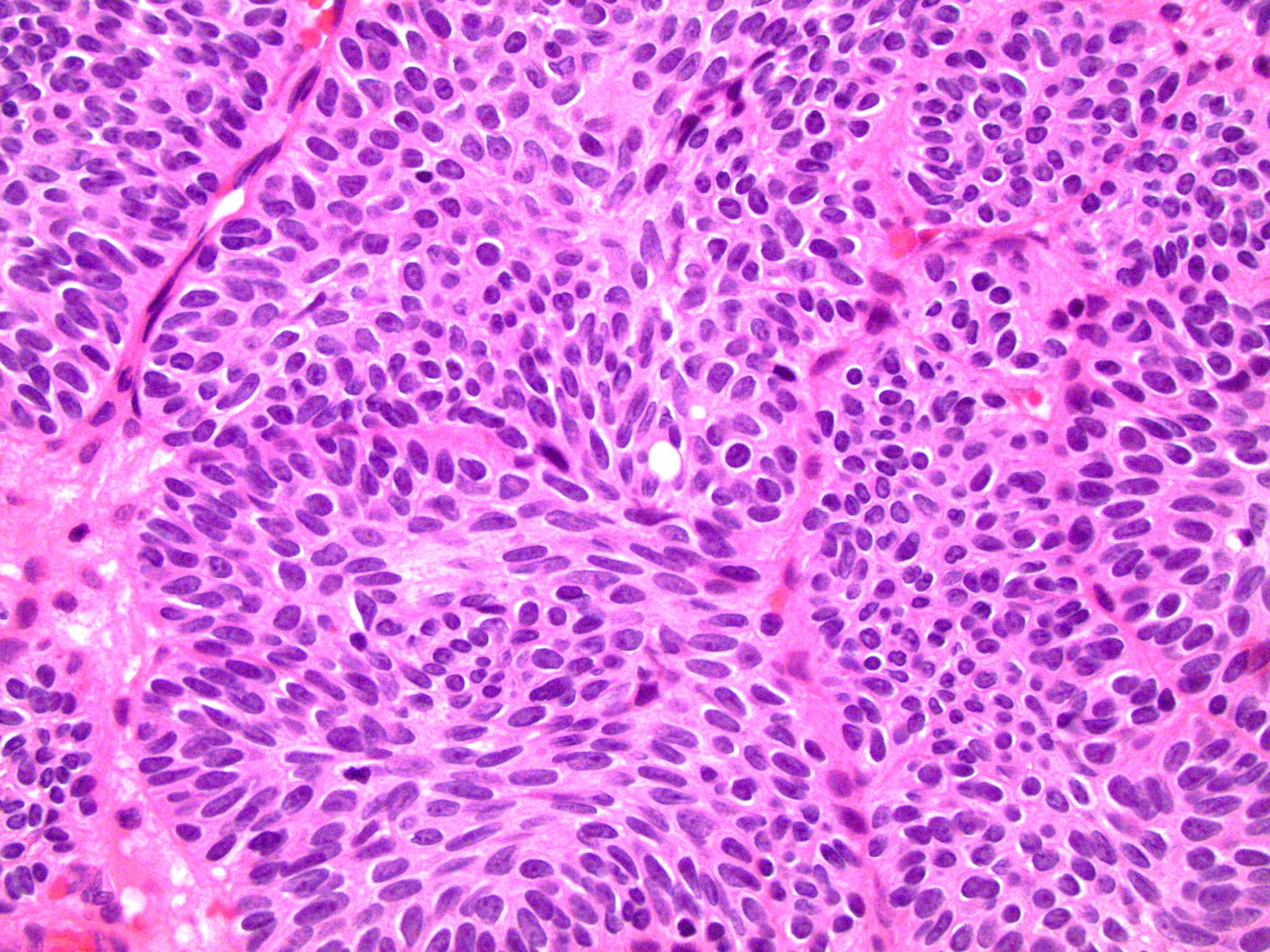
In general, papillary urothelial cancers have a better prognosis than other types of bladder cancer. Your specific outlook depends on the stage and grade of your cancer. High-grade cancers can spread. Low-grade papillary cancers are less likely to spread. Papillary cancers can also return after theyve been treated.
Read Also: What Causes A Cyst On Your Bladder
Cancer That Has Spread To The Bladder
Sometimes cancer that has started elsewhere in the body can spread to the bladder. This can happen with prostate, rectum, ovary, cervix and womb cancer for example.
Cancers that have spread from somewhere else in the body are called secondary cancers. The cancer cells are the same type as the first cancer. So is the treatment.
If you have cancer that has spread to the bladder, you need to go to the section about your primary cancer.
-
Cancer and Its Management J Tobias and D HochhauserWiley Blackwell, 2015
-
A M Kamat and othersThe Lancet, 2016. Volume 388, Pages 276 -2810
-
AJCC Cancer Staging Manuel American Joint Committee on CancerSpringer, 2017
-
Bladder cancer: diagnosis and management of bladder cancerNational Institute of Health and Clinical Excellence, 2015
-
Bladder Cancer
Treatment Of Bladder Cancer By Stage
Most of the time, treatment of bladder cancer is based on the tumors clinical stage when it’s first diagnosed. This includes how deep it’s thought to have grown into the bladder wall and whether it has spread beyond the bladder. Other factors, such as the size of the tumor, how fast the cancer cells are growing , and a persons overall health and preferences, also affect treatment options.
Don’t Miss: How To Take Care Of A Bladder Infection At Home
Non Muscle Invasive Bladder Cancer
In non muscle invasive bladder cancers, the cancer is only in the lining of the bladder. It has not grown into the deeper layers of the bladder wall. Non muscle invasive bladder cancer is also called superficial bladder cancer, or early bladder cancer.
Early bladder cancer usually appears as small growths, shaped like mushrooms. These grow out of the bladder lining. This is called papillary bladder cancer. Your surgeon can remove these growths and they may never come back.
But some types of early bladder cancer are more likely to come back. These include carcinoma in situ and high grade T1 tumours. T1 stands for the size of the tumour.
Carcinoma in situ
Unlike other early bladder cancers, areas of CIS are flat. They do not grow out of the bladder wall. In CIS the cancer cells look very abnormal and are likely to grow quickly. This is called high grade. It is more likely to come back than other types of early bladder cancer.
High grade T1 tumours
T1 tumours are early cancers that have grown from the bladder lining into a layer underneath, called the lamina propria. High grade T1 tumours are early cancers, but they can grow very quickly.
Risk groups
Doctors divide early bladder cancer into 3 risk groups. These risk groups describe how likely it is that your cancer will spread further or come back after treatment. Your risk group depends on several factors including the size of the tumour , what the tissue looks like under the microscope and type of bladder tumour.