Symptoms Of Pelvic Organ Prolapse
Pelvic organ prolapse symptoms include:
- a feeling of heaviness around your lower tummy and genitals
- discomfort or numbness during sex
- problems peeing such as feeling like your bladder is not emptying fully, needing to go to the toilet more often, or leaking a small amount of pee when you cough, sneeze or exercise
Sometimes pelvic organ prolapse has no symptoms and is found during an internal examination carried out for another reason, such as cervical screening.
My Bladder Has Fallen And I Cant Get Up Why Didnt Anyone Tell Me About Cystocele
When I was pregnant with my first child, I read everything I could. But, one thing no one told me was that one possible side effect of childbirth could be that my bladder may someday fall out of its normal resting spot inside my body.
Now before I send any of my pregnant readers into a tizzy, please note that this condition, known as cystocele, is fairly uncommon, especially among younger women. But, if you have ever needed a reason to kegel, keep reading.
OK. . .all clear?
Heres the scoop:
It was another ordinary night in the Fairly Odd household in spring 04. Fairly Odd Father was enjoying a night out with the boys to see the Boston Bruins. I was four months pregnant with my third child. Belly was three and Jilly had just turned a year old.
I decided to give the girls a bath, so I got the water in the tub ready. But, as I lifted them into the tub, I felt an odd sensation. It was if something was sliding out of me. Not painful, just not right. I had visions of me birthing my baby right then and there, on the bathroom floor. I thought about an ex-coworker who told the story of how her mother knew she was about to birth her twins when she looked down and saw a leg coming out. I hope I dont see a leg was all my brain could muster.
I then reached down and pushed something back up into my body. Something squishy and fleshy and not a baby leg. I suppose I should be so very thankful of that fact.
I answered his questions:
Choose A Minimally Invasive Gyn Specialist For Your Pelvic Organ Prolapse Surgery
Specialists have a high volume of patients, making for a high level of experience. Learn more about your options. There is nothing more important than being well-informed about possible treatments and what they entail. CIGC surgeons Dr. Paul MacKoul, MD and Dr. Natalya Danilyants, MD assess your individual case, what you are experiencing and whether or not you are planning to have children, and then recommend the best possible treatment options.
Read Also: How To Fix Bladder Leakage After Pregnancy
Prolapsed Bladder Symptoms In Men:
- Male urinary dysfunction: This condition can involve leaking urine after peeing, frequent urination and other bladder and bowel issues.
- Erectile Dysfunction : ED is when men cant get or maintain an erection during sex. Sometimes pelvic muscle tension or pain can contribute to this issue.
- Prostatitis: Pelvic floor dysfunction and prolapse symptoms closely resemble prostatitis, which is an infection or inflammation of the prostate. Prostatitis can have many causes including bacteria, sexually transmitted infections or trauma to the nervous system.
- A sense that something is falling out
- Trouble emptying your bowel or bladder completely
- Urine leakage, frequency, chronic urinary tract infections, difficulty urinating
- Difficult bowel movements or trapping of stool
When To Call A Professional
Prolapse of the pelvic organs is generally a nonthreatening problem. You should contact your physician for an evaluation if you are having bothersome symptoms, and you suspect you might have this problem. It is also important to report changes in urinary symptoms to your doctor, since urinary infections are a possible complication of prolapse.
Recommended Reading: Women’s Bladder Falling Out
Diagnosis Of Bladder Prolapse
Bladder prolapse is diagnosed by:
- medical history including checking for possible risk factors
- physical vaginal examination to allow assessment of the degree of prolapse, pelvic floor muscle function, presence of any other prolapse and other abnormalities in the pelvis, such as tumours or masses.
Dont Miss: Colon Cancer And Bladder Problems
How Is Vaginal Prolapse Treated
Vaginal prolapse treatment can vary depending on the severity of your prolapse. In some cases, your healthcare provider may want to just watch it over time to make sure it doesnt get worse.
There are nonsurgical and surgical treatment options for vaginal prolapses. There are a few things your healthcare provider will take into account when forming a treatment plan. These can include:
- Your general health and if you have any other serious medical conditions.
- The severity of your prolapse.
- If you want to have children in the future.
- If you want to have penetrative sex in the future.
Its important to have an open and honest conversation with your healthcare provider about these topics. Talk to your healthcare provider about any questions or concerns you have regarding these treatments.
Nonsurgical treatments are typically used as a first option and work best with minimal or mild prolapses. Specific treatment options can include:
For more severe cases, surgery to correct vaginal prolapse can be an option. These options include:
Also Check: How To Heal An Overactive Bladder
Tests For Bladder Prolapse
Tests that may be carried out to confirm or reject a diagnosis of bladder prolapse, depending on your symptoms, are:
- pelvic ultrasound to exclude any masses or cysts putting pressure on the bladder
- urodynamics a test of bladder function and to assess different types of incontinence
- a bladder scan to measure residual urine urine left in the bladder after emptying
- a midstream urine test to exclude urinary tract infection
- magnetic resonance imaging in some cases.
Bladder Prolapse At A Glance
- Bladder prolapse occurs when the hammock of pelvic floor muscles that support the bladder weakens and the bladder drops out of its proper position.
- Bladder prolapse, also called cystocele, commonly occurs in women due to age, injury or childbirth.
- Treatment ranges from lifestyle changes to medications and surgery.
You May Like: Why Do You Lose Bladder Control
What Are The Complications Of A Cystocele
A cystocele may put pressure on or lead to a kink in the urethra and cause urinary retention, a condition in which you are unable to empty all the urine from your bladder. In rare cases, a cystocele may result in a kink in the ureters and cause urine to build up in the kidney, which can lead to kidney damage.
Recommended Reading: How To Help A Weak Bladder Naturally
When To Contact A Doctor
A person may not need to consult a doctor right away if symptoms are mild or do not cause issues. Someone may only need to contact a doctor if their symptoms worsen.
People should consider consulting a medical professional if their symptoms are moderate to severe and causing issues with their daily lives. A doctor can help diagnose and provide advice on treatment for the prolapse.
You May Like: Home Remedies For Bladder Infection In Women
What Are Treatments For A Prolapsed Bladder
Nonsurgical Treatment
Nonsurgical treatment consists of conservative management and the use of mechanical devices.
Behavioral therapy and pelvic floor muscle exercise are conservative therapies for management of bladder prolapse. The goal of conservative treatment is the reduction of symptoms, prevention of worsening pelvic organ prolapse, increased support of the pelvic floor musculature, and avoiding or delaying surgery. Behavioral therapy includes reducing risk factors such as treating constipation, weight loss if obese, and discontinuing smoking if COPD/cough, etc. PFME are muscle exercises to strengthen the pelvic floor muscles. The contractions should be held for two to 10 seconds and should be performed regularly several times per day. A set of 10 sustained contractions for a duration of about 20 minutes should be performed two to three times per day. This form of therapy is suitable for mild to moderate pelvic organ prolapse.
How Do Health Care Professionals Diagnose A Cystocele

To diagnose a cystocele, health care professionals ask about your symptoms and medical history and perform a physical exam, including a pelvic exam to check your lower abdomen. You may be asked to stand during part of the exam, which may feel awkward but allows your health care professional to determine the severity of your cystocele. Your health care professional may also order medical tests to determine how advanced the cystocele is or to help find or rule out other problems in your urinary tract or pelvis.
Recommended Reading: Tuberculosis To Treat Bladder Cancer
Exams And Tests For A Prolapsed Bladder
For less obvious cases, the doctor may use a voiding cystourethrogram to help with the diagnosis. A voiding cystourethrogram is a series of X-rays that are taken during urination. These help the doctor determine the shape of the bladder and the cause of urinary difficulty. The doctor may also test or take X-rays of different parts of the abdomen to rule out other possible causes of discomfort or urinary difficulty.
After diagnosis, the doctor may test the nerves, muscles, and the intensity of the urine stream to help decide what type of treatment is appropriate.
A test called urodynamics or video urodynamics may be performed at the doctor’s discretion. These tests are sometimes referred to as “EKGs of the bladder”. Urodynamics measures pressure and volume relationships in the bladder and may be crucial in the decision making of the urologist.
Cystoscopy may also be performed to identify treatment options. This test is an outpatient office procedure that is sometimes performed on a television screen so the person can see what the urologist sees. Cystoscopy has little risk and is tolerable for the vast majority of people.
Prolapsed Bladder Care At Home
For mild-to-moderate cases of prolapsed bladder, the doctor may recommend activity modification such as avoiding heavy lifting or straining. The doctor may also recommend Kegel exercises. These are exercises used to tighten the muscles of the pelvic floor. Kegel exercises might be used to treat mild-to-moderate prolapses or to supplement other treatments for prolapses that are more serious.
You May Like: How To Stage Bladder Cancer
How Can I Prevent Pelvic Organ Prolapse
Researchers are studying ways to prevent pelvic organ prolapse. The following steps may reduce your risk of getting a pelvic floor problem:
- Maintain a healthy weight or lose weight . Women who have overweight or obesity are more likely to have pelvic floor problems.
- Choose foods with fiber. Fiber helps prevent constipation and straining during bowel movements. Preventing constipation may reduce the risk of some pelvic floor disorders.
- Do not smoke. Smoking can lead to chronic cough, which puts stress on the pelvic floor muscles.
What Are Proper Lifting Techniques And How Do They Help Prevent A Prolapse
When you lift something heavy, you can strain your muscles. This strain can lead to a pelvic organ prolapse. By following a few tips, you can lower your risk of prolapse.
- Dont lift alone: When you have something thats oddly shaped or very large, get help lifting it.
- Check your footing: Make sure you have a good footing before lifting something.
- Lift with your legs: When you pick something up thats lower than the level of your waist, keep your back straight and bend at your knees and hips. Dont bend forward at the waist with your knees straight.
- Use a wide stance: Keep your feet apart and firmly on the ground when you lift something.
- Dont jerk or twist when you lift something: Make sure that you straighten your knees in a steady motion and dont jerk the object up.
- Reposition objects before lifting: If youre lifting an object from a table, slide it to the edge so that you can hold it close to your body.
- Hold packages close to your body: Keep your arms bent, your stomach muscles tight and hold the object closer to the core of your body.
- Lower objects in the same way you picked them up: Place your feet apart, tighten your stomach muscles and bend at your hips and knees to lower an object.
Recommended Reading: T1 Low Grade Bladder Cancer
What Causes Pelvic Organs To Prolapse
Pelvic organs can start to fall out of place due to damage of the ligaments and muscles which support the pelvic organs. Damage can arise from:
- Pregnancy and childbirth which are considered major factors
- Conditions that cause excessive pressure on the pelvic floor like obesity, persistent coughing, heavy lifting and chronic constipation
- It may also occur as a result of other medical conditions that can damage the muscles, nerves and ligaments in the pelvis. In rare cases, an abdominal or pelvic mass or tumour can cause a this or make it worse
Complication Rates By Type Of Sling
Before undergoing bladder sling surgery, women should ask their doctors about the technique they plan to use. Complication rates may vary depending on the type of mesh sling and technique.
A 2010 study of bladder sling procedures by Z. Chen and colleagues published in Urologia analyzed the outcomes of 187 women who received bladder slings to treat stress urinary incontinence. Authors found that transobturator vaginal tape inside-out and transobturator vaginal tape out-inside are simpler techniques with fewer complications compared to tension-free vaginal tape .
Women who used TVT had an average hospital stay of five days versus about two days for the TOT group.
The complication rate in the study was:
- 15.6 percent for tension-free vaginal tape
- 9.20 percent for transobturator vaginal tape inside-out
- 8.90 percent for transobturator vaginal tape out-inside
Complications from the procedures included discomfort with urinating, bleeding outside blood vessels and dysfunction of lower limbs. TVT was the only procedure associated with bladder perforation. Despite the complication rate, doctors found the slings safe.
The three tension-free urethral suspension techniques have similar efficacy, all of them are safe and effective procedures for the treatment of female SUI, authors wrote.
Also Check: Survival Rate For Bladder Cancer Stage 4
Causes Of A Prolapsed Bladder
The following factors are commonly associated with causing a prolapsed bladder:
- Childbirth: This is the most common cause of a prolapsed bladder. The delivery process is stressful on the vaginal tissues and muscles, which support a womanâs bladder.
- Straining: Lifting heavy objects, straining during bowel movements, having a long-term condition that involves coughing, or having long-term constipation may damage the muscles of the pelvic floor.
Do I Need Pelvic Organ Prolapse Surgery
Depending on the severity of your pelvic organ prolapse symptoms, minimally invasive GYN surgery may be the best treatment, said Dr. Paul MacKoul, MD, The Center for Innovative GYN Care. Some patients find that their symptoms are manageable and prefer not to treat them. Others decide that surgical management is the best option for them as conservative treatments are not effective for long-term relief. However, surgery is typically delayed until women are finished with childbearing.
Women with symptoms for whom conservative management options are unsuccessful can seek a minimally invasive pelvic organ prolapse surgery. Surgical outcome can depend upon the severity of symptoms, extent of prolapse, and the patients expectations.
Also Check: Symptoms Of Bladder Prolapse After Hysterectomy
Who Is More Likely To Have A Cystocele
A cystocele can affect women of any age, but your chances of developing a cystocele increase with age because muscles and tissues often become weaker over time. Other factors that increase your risk of having a cystocele include
- giving birth vaginally
- having a family history of pelvic organ prolapse
Vaginal Extrusion And Erosion
Additionally, Gomes and colleagues found urethral erosion happened after less than 1 percent of sling surgeries.
A pelvic exam revealed mesh extrusion.
In some cases, conservative management of erosion may be possible. For example, some surgeons may prescribe topical estrogen cream to help vaginal tissues heal.
Don’t Miss: What To Expect After Bladder Sling Surgery
After Treatment Of Prolapse Bladder
Nonsurgical therapy may be all that is required to successfully treat a prolapsed bladder in mild situations.
Some women will require a second procedure if the first failed, the cystocele resurfaced, or another pelvic floor issue developed. Women who are older, smokers, diabetics, or have had a hysterectomy are more prone to have problems.
Additionally, Gomes and colleagues found urethral erosion happened after less than 1 percent of sling surgeries.
A pelvic exam revealed mesh extrusion.
In some cases, conservative management of erosion may be possible. For example, some surgeons may prescribe topical estrogen cream to help vaginal tissues heal.
How To Diagnose And Treat A Prolapsed Bladder
This article was medically reviewed by Lacy Windham, MD. Dr. Windham is a board certified Obstetrician & Gynecologist in Tennessee. She attended medical school at the University of Tennessee Health Science Center in Memphis and completed her residency at the Eastern Virginia Medical School in 2010, where she was awarded the Most Outstanding Resident in Maternal Fetal Medicine, Most Outstanding Resident in Oncology, and Most Outstanding Resident Overall.There are 12 references cited in this article, which can be found at the bottom of the page.wikiHow marks an article as reader-approved once it receives enough positive feedback. In this case, 96% of readers who voted found the article helpful, earning it our reader-approved status. This article has been viewed 112,458 times.
Also Check: What Does It Mean When You Have A Weak Bladder
What Is A Prolapsed Bladder
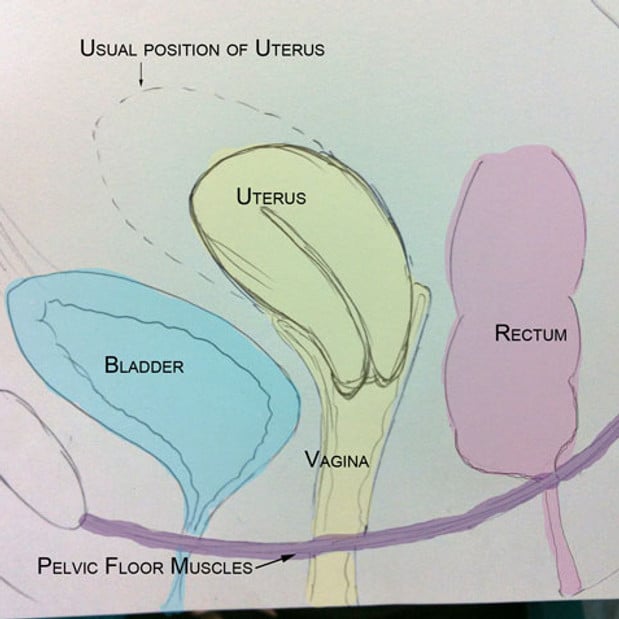
Pelvic organ prolapse is a surprisingly common condition. In fact, its estimated that about half of women over 50 have some level of prolapse. The pelvic floor is a web of muscles and tissues that supports your pelvic organs, including the bladder, bowel, and uterus. When these muscles and tissues become weakened or damaged, one or more of these pelvic organs can drop or collapse, causing uncomfortable symptoms.
While any of the organs listed above can drop, the most common type of prolapse is a dropped bladder, also known as a cystocele.
Recommended Reading: Can You Have A Bladder Infection Without Symptoms