Will I Need Surgery To Treat Pelvic Floor Dysfunction
There is not a surgery to treat pelvic floor dysfunction because it is a problem with your muscles. In rare circumstances, when physical therapy and biofeedback fail to work, your provider might recommend you see a pain injection specialist. These doctors specialize in localizing the specific muscles that are too tense or causing pain, and they can use a small needle to inject the muscle with numbing medication and relaxing medication. This is called trigger point injection.
Prevalence Of Bladder And Bowel Dysfunction In Toilet
- Division of Nephrology, Department of Pediatrics, ICMR Center for Advanced Research in Nephrology, All India Institute of Medical Sciences, New Delhi, India
Introduction: Urinary tract infection in children leads to renal scarring in 1015% of patients. Urinary tract anomalies and bladder and bowel dysfunction are documented risk factors for recurrent UTIs. Estimates of baseline prevalence of BBD in children with UTI will help the clinician in the management strategy. Hence, a systematic review and meta-analysis was conducted to estimate the pooled prevalence of BBD.
Methods: MEDLINE, EMBASE, and CENTRAL databases were searched for articles related to UTI, primary vesicoureteral reflux , and BBD. We included studies that provided prevalence of BBD in toilet-trained patients aged 118 years with UTI and/or VUR. BBD was defined based on clinical history or questionnaire or urodynamic studies. Two authors independently reviewed, assessed, and abstracted data from studies. Pooled prevalence was calculated based on a random effects model.
Almost half of the patients with primary VUR have BBD, and its presence increases the risk of recurrent UTIs. Trends of high BBD prevalence were also observed in patients presenting with UTI without VUR. These prevalence estimates suggest that all toilet-trained children presenting with UTI with or without VUR should be assessed for BBD, which will help in their further management.
What You Need To Know
- Issues with urinating or passing stools are referred to as bladder and bowel dysfunction.
- Bladder and bowel problems often originate with nerve or muscle dysfunction, as these systems control the flow of urine and the release of stool.
- Other health issues may cause bladder and/or bowel dysfunction, including medicinal side effects, stress, neurologic diseases, diabetes, hemorrhoids and pelvic floor disorders.
- Therapy and management for these conditions can range from dietary changes and exercise to electrical stimulation and surgery depending on individual diagnosis.
Bladder or bowel incontinence means a problem holding in urine or stool. You may have unwanted passage of urine or stool that you cant control. These conditions can be stressful to deal with. But dont feel embarrassed about talking to your healthcare provider. They are used to dealing with these issues, and can help you manage the problem.
Don’t Miss: Can Bladder Cancer Be Seen On Ultrasound
Continence Problems And Bladder Or Bowel Issues
Incontinence and continence problems are symptoms of bladder or bowel dysfunction. They tell you that something is not quite right. Pelvic floor muscle weakness is a common cause of these symptoms. Changes to the nerves controlling the bladder, bowel or pelvic floor can also result in loss of control.Sometimes, other health problems such as diabetes, stroke, Parkinsons disease or multiple sclerosis can cause bladder or bowel control problems.
What Else Causes Bladder Control Problems In Women
Certain life events and health problems can lead to stress incontinence in women by weakening the pelvic floor muscles
- pregnancy and childbirth
- menopause
Weak pelvic floor muscles can make it hard for your bladder to hold urine in during stress incontinence. Stress incontinence occurs when an actioncoughing, sneezing, laughing, or physical activityputs pressure on your bladder and causes urine to leak. A weak pelvic floor can also cause fecal incontinence, or bowel control problems.
You May Like: Can Bladder Infection Cause Cramps
How Can Bowel Function Be Affected With Multiple Sclerosis
Bowel dysfunction is also a common symptom for patients with MS. One study of 77 patients with clinically definite MS showed that bowel problems are not associated with bladder dysfunction, patient’s age, degree of disability, or duration of disease.
The most common bowel complaint from a person with MS is constipation, but the most distressing bowel complaint is probably that of involuntary bowel/fecal incontinence. Because MS interrupts or slows the transmission of signals to and from the brain, the electrical impulses to the muscles that are involved in emptying your bowel can become disrupted.
Depending on your particular bowel problem, helpful suggestions can be made. General interventions for bowel dysfunction include:
- Education about the causes of bowel dysfunction
- Encouraging dietary changes to include more fiber and fluid
- Consulting with your healthcare provider to adjust medication regimens that may be contributing to bowel dysfunction
- Establishing a regular bowel routine, individualized to the patient
- Encouraging regular physical activity
Bladder and bowel symptoms are common in MS and can be effectively managed. Speak with your healthcare provider about what you can do to help keep these symptoms under control.
What Causes Bladder Or Bowel Incontinence
Many conditions may affect the nerves and muscles that control the bladder and bowel.
Bladder incontinence can be caused by things such as:
-
Damage to nerves in sphincter muscles
-
Holding urine in too long , which can damage the bladder
-
Having to urinate many times during day and night, often urgently
-
Diarrhea
Bowel incontinence can be caused by things such as:
-
Diarrhea
-
Damage to the nervous system from disease or injury
-
Vaginal childbirth
Also Check: How To Relax The Bladder Naturally
Living With Bowel Or Bladder Incontinence
There is no single, right way to cope with bladder or bowel incontinence. The challenge is to find what is best for your situation, so you can get the help you need and return to a normal daily life. Talk with your health care team if you notice a change in bowel or bladder habits, and about the best ways to manage incontinence, if it is a problem. You might find it helpful to talk with other people who are dealing with incontinence, too. Ask a member of your cancer care team about support groups in your area.
Here are some things you can do that may help make incontinence less of a problem:
- Empty your bladder every 3 to 4 hours while awake, to avoid accidents.
- Empty your bladder before bedtime or before strenuous activity.
- Limit drinks with caffeine, or and avoid alcohol and citrus juices, which can irritate the bladder and make you have to go more often.
- Avoid hygiene products that may irritate you Women should avoid feminine spray or over-the-counter vaginal suppositories.
- Because belly fat can push on the bladder, avoiding weight gain or losing needed weight sometimes helps improve bladder control.
- Avoid tobacco use which can cause coughing and bladder irritation due to harmful substances in tobacco products.
- Talk to your doctor about all medicines, vitamins, herbs, and supplements youre taking. Some may affect urine control.
What The Caregiver Can Do
- Encourage or help the patient with appropriate skin care after using the bathroom. Use warm water and pat the area dry.
- Help the patient keep a diary that records specific foods or drinks that may affect how frequently the patient goes to the bathroom.
- Help the patient maintain a bladder or bowel plan.
- Encourage the patient to go to the bathroom at consistent time frames during the day, like after a meal.
- Encourage regular daily exercise, as permitted by the health care team.
Don’t Miss: Natural Supplements For Bladder Health
What Makes Pelvic Floor Dysfunction Worse
It can take several months of routine bowel or urinary medications and pelvic floor physical therapy before symptoms of pelvic floor dysfunction start to improve. The most important part of treatment is to not give up. Forgetting to take your medications every day will cause your symptoms to continue and possibly get worse. Also, skipping physical therapy appointments or not practicing exercises can slow healing.
Any activity that increases the tension or pain in your pelvic floor muscles can cause your symptoms to get worse. For example, heavy weightlifting or repetitive jumping can increase your pelvic floor tension and actually worsen symptoms.
If you have problems with constipation due to hard bowel movements or abdominal bloating and gas pain, then you should consult with your doctor and watch your diet closely. Its important to drink plenty of water daily and eat a healthy diet. Foods that are high in fiber, or fiber supplements, may worsen your bloating symptoms and gas pains. These foods should be avoided if your symptoms get worse.
When To Get Medical Advice
See a GP if you have difficulty controlling your bowels. Do not be embarrassed about talking to someone about it.
Remember that:
- it’s not something to be ashamed of
- it’s common and GPs are used to seeing people with it
- it’s not something you have to put up with
- it will probably not get better on its own
- it can be treated
If you’d prefer not to see a GP, you may be able to make an appointment at an NHS continence service instead. Call your local hospital for details of your nearest service.
Read Also: Bladder Sling Lawsuit Statute Of Limitations
Treatment For Overactive Bladder
At the time of visit your physician will perform a thorough history and physical to evaluate for OAB, and find a possible cause. He/She may also order some tests to confirm the diagnosis such as urinalysis, post void residual, urodynamics and a voiding diary. Once the diagnosis is confirmed, he or she will discuss life style changes, exercises, and possibly medications.
If those are not effective, or cause side effects, options such as Peripheral Tibial Nerve Stimulation , Sacral Nerve Modulation , and Botox injection will be discussed. All these have their pros and cons and these will be presented to you so that you may make an informed decision. Dr. Lotenfoe is fully qualified and experienced to perform these procedures.
A brief word on Sacral Nerve Modulation : Initially only a test is performed to see if you have a good result. A small electrode is placed next to the nerve controlling the bladder. This procedure is done outpatient under local anesthesia. There will be test period of usually a week or so where the electrode will induce tiny electrical pulses to the nerve. If you have a good result, a small electronic device is implanted under the skin for continued modulation. Dr. Lotenfoe has performed many of these procedures over the years with high success rates.
What Causes You To Lose Control Of Your Bladder And Bowel

Causes of bladder and bowel incontinence can include damage to nerves, holding urine for too long, having an overactive bladder, having diarrhea or constipation, vaginal childbirth, pelvic organ prolapse, side effects of medicine, stress, neurological conditions diabetes, infection or problems with the pelvic floor.
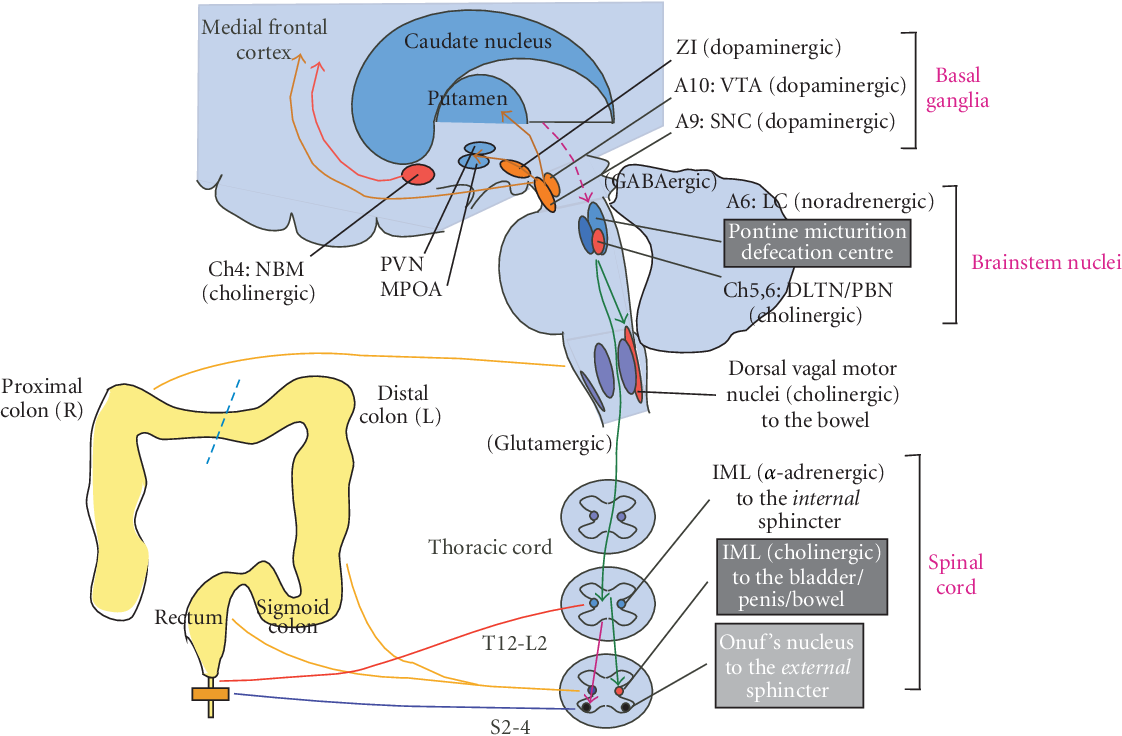
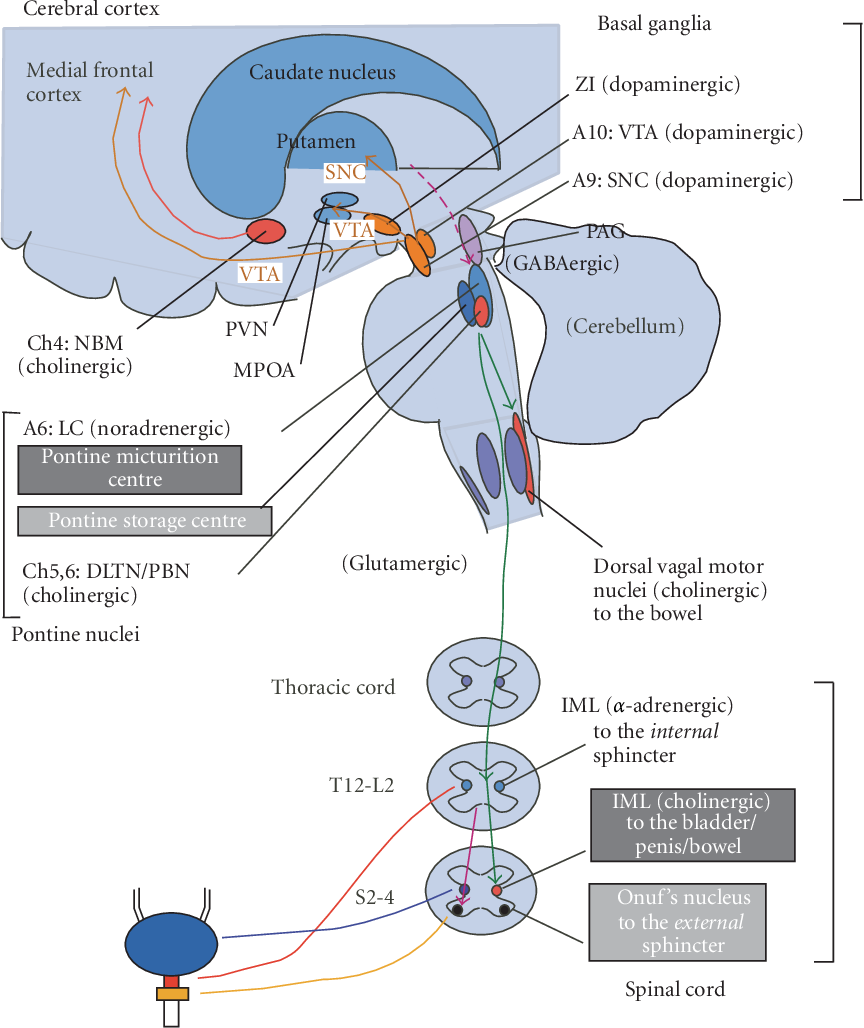
In a normally functioning bladder and bowel, nerves tell certain muscles when to tighten and when to relax. The brain tells the nerves via the spinal cord what to do. Sphincter muscles control the holding of urine or stool and the nerves tell them when to contract and when to relax.
Also Check: Can Anxiety Cause Overactive Bladder
Study Selection And Characteristics
On the basis of patients enrolled, we categorized studies into two groups: nine studies of patients with UTI and without primary VUR and 30 studies of patients with primary VUR . Three studies were included in the final systematic review as they reported data on rates of recurrence of UTI , and one study by Chung et al. provided data on constipation .
How Is Pelvic Floor Dysfunction Diagnosed
Your healthcare provider will usually start by asking about your symptoms and taking a careful medical history. Your provider may ask you the following questions:
- Do you have a history of urinary tract infections?
- If youre female, have you given birth?
- If youre female, do you have pain when you have sex?
- Do you have interstitial cystitis or irritable bowel syndrome ?
- Do you strain to pass a bowel movement?
Your provider may also do a physical exam to test how well you can control your pelvic floor muscles. Using their hands, your provider will check for spasms, knots or weakness in these muscles. Your provider may also need to give you an intrarectal exam or vaginal exam.
You may also be given other tests including:
Don’t Miss: Complete Loss Of Bladder Control
How To Approach Your Gp About Your Bowel Problems
It is never too late to get help with your bowel problems. If you would like some advice on how to approach your GP regarding your bowel problem you may find our Advice Sheet helpful. It also includes information on tests that your GP may recommend you have done. To download, please click on this link Bowel Advice Sheet.
Types Of Bladder Control Problems
Urinary incontinence and continence problems may include:
- stress incontinence leakage of small amounts of urine with exertion. Causes include childbirth, being overweight and prostate surgery
- urge incontinence leakage following a sudden urge to urinate. Causes include stroke, enlarged prostate gland and Parkinsons disease, but often the cause is unknown
- overflow incontinence leakage because the bladder does not empty well and overfills. Causes include multiple sclerosis, an enlarged prostate gland and diabetes
- functional incontinence leakage of urine because a person was unable to get to or use the toilet due to a physical disability, a barrier in their environment or because of an intellectual or memory problem. Causes include dementia and poor mobility.
Also Check: Slow Urine Flow When Bladder Is Full
What Does Pelvic Floor Dysfunction Feel Like
Several symptoms may be a sign that you have pelvic floor dysfunction. If you have any of these symptoms, you should tell your healthcare provider:
- Frequently needing to use the bathroom. You may also feel like you need to force it out to go, or you might stop and start many times.
- Constipation, or a straining pain during your bowel movements. Its thought that up to half of people suffering long-term constipation also have pelvic floor dysfunction.
- Straining or pushing really hard to pass a bowel movement, or having to change positions on the toilet or use your hand to help eliminate stool.
- Leaking stool or urine .
- Feeling pain in your lower back with no other cause.
- Feeling ongoing pain in your pelvic region, genitals or rectum with or without a bowel movement.
Prevalence Of Bladder And Bowel Dysfunction Among Patients With Urinary Tract Infection Without Primary Vesicoureteral Reflux
A total of nine studies comprising of 920 patients reported prevalence of BBD in toilet-trained children presenting with UTI without VUR . The pooled prevalence of BBD in patients with UTI was 41% . Owing to high heterogeneity , random effects estimates were used. Three studies reported separate data on prevalence of BBD in girls, at 41% . None of the studies provided separate information on prevalence of BBD in boys. On a subgroup analysis, the prevalence of BBD was higher in prospective studies as compared with retrospective studies .
Figure 2. Prevalence of bladder dysfunction in children with urinary tract infection without primary vesicoureteral reflux .
Read Also: Why Am I Losing Control Of My Bladder
Managing Bladder Or Urinary Incontinence
Sometimes urinary incontinence can last a short time, depending on what’s causing it. But sometimes incontinence can be long-term and uncomfortable, making some everyday activities difficult to manage.
Your health care team will ask you questions to determine the type of bladder incontinence you might have. Then, you might need tests to verify the type and learn the cause of it which will help them know the best way to manage it.
- Pelvic floor muscle strengthening may be recommended. A physical therapist that specializes in pelvic floor muscle exercises can help. This might help muscle strength and bladder control get better by doing exercises that tighten and relax muscles that control the flow of urine.
- Bladder training canhelp manage how often you need to urinate throughout the day, by assigning certain time intervals to empty your bladder.
What Are Some Bladder Management Points To Remember If I Have Multiple Sclerosis
- Adequate fluid intake is 1½-2 quarts of fluid a day. The urge to urinate comes about 1½ -2 hours after drinking something.
- Caffeine, aspartame, and alcohol are all bladder irritants.
- Smoking also is irritating to the bladder.
- Limiting fluid is harmful.
- It is not normal to leak urine, wake up more than once at night to urinate, or to have frequent urinary tract infections.
- Bladder infections in people with MS may result in an increase in MS symptoms, spasticity, and fatigue.
Plan of action
- Drink fluids all at once . If you sip, sip, sip you will feel the urge to urinate frequently. Try to go about 1½ to 2 hours after you drink.
- Stop drinking fluids about 2 hours before bedtime urinate right before bedtime.
- If you tend to get frequent bladder infections you are probably not emptying your bladder completely.
- Taking cranberry pills may keep your urine more acidic and decrease the bacteria in your urine.
Also Check: Why Do I Keep Getting Bladder Infections After Intercourse
Experimental Use Of Botox
UW Health doctors work continuously to find new ways to treat bladder problems. The use of Botox to treat overactive bladder is one example of how we put research to work.
In this treatment, your doctor injects Botox into your bladder muscles. This relaxes the muscles, reducing your urge to urinate. This treatment works particularly well for people with a bladder condition caused by nervous system injury.
Meet our team