How Anticholinergic Bladder Medications Work
Anticholinergic drugs are often prescribed to treat OAB. These drugs work by relaxing your bladder muscles. They also help prevent urine leaks by controlling bladder spasms.
Most of these drugs come as oral tablets or capsules. They also come in transdermal patches and topical gels. Most are only available as prescriptions, but the patch is available over the counter.
Oxybutynin is an anticholinergic drug for overactive bladder. Its available in the following forms:
- oral tablet
- transdermal patch
- topical gel
You take this drug on a daily basis. Its available in several strengths. The oral tablet comes in immediate-release or extended-release forms. Immediate-release drugs release into your body right away, and extended-release drugs release into your body slowly. You may need the take the immediate-release form up to three times per day.
Dont Miss: Best Pills For Bladder Infection
What Is Overactive Bladder
Overactive bladder is the term used to describe the symptom complex of urinary urgency, usually accompanied by frequency and nocturia, with or without urge urinary incontinence, in the absence of urinary tract infection or other obvious pathology.1
Epidemiological studies in North America have reported a prevalence of overactive bladder in women of 16.9%, and the prevalence increases with agefrom 4.8% in women under 25 years to 30.9% in those aged over 65 years.2 Prevalence data from Europe are similar, with frequency the most commonly reported symptom , and 54% reporting urgency and 36% urge incontinence.3
The symptoms of overactive bladder are most likely due to involuntary contractions of the detrusor muscle during the filling phase of the micturition cycle abnormalities in afferent sensation may also play a role. Detrusor overactivity1 is mediated by acetylcholine induced stimulation of muscarinic receptors
Percutaneous Tibial Nerve Simulation
A less invasive option called percutaneous tibial nerve stimulation is also available. It only takes about half an hour per session to perform and is usually done in a doctors office.
In PNTS, a needle electrode is inserted near the ankle that delivers electrical pulses to the tibial nerve. This nerve is linked directly to the sacral nerve.
As in SNS, these electrical pulses help block inappropriate bladder signaling.
Read Also: Botox Injection For Bladder Incontinence
You May Like: Depend Adult Bladder Control Pads
Are Claims For Newer Drugs For Overactive Bladder Warranted
Two previous Therapeutics Letters on drugs for overactive bladder concluded that the antimuscarinic drugs had limited short-term potential symptomatic benefit and significant risk of adverse effects .1, 2 This Letter compares drugs to one another, including newer drugs introduced since 2007, when our most recent Letter on this topic was published.2
Search Strategy And Selection Criteria
This systematic review was done according to the PRISMA statement . A review protocol was elaborated, which is available on file with the authors. To identify randomized controlled trials of antimuscarinics versus placebo , we started with the recent Cochrane review by Nabi et al. and a literature search update from June 2005 to November 2007 kindly provided by the Cochrane Incontinence Review Group according to their previously published search strategy . Head-to-head comparative trials without a placebo arm were identified from the two recent meta-analysis by Chapple et al. and by Novara et al. . In addition, we searched reference lists and conference abstracts by hand, checked relevant reviews, book chapters, and contacted manufacturers and trialists. The search strategies are available on request.
Two investigators independently assessed reports for eligibility. To be included, studies had to be randomized controlled trials comparing at least one antimuscarinic for treating OAB with placebo or with another antimuscarinic. All currently used antimuscarinics were included, i.e. darifenacin, fesoterodine, oxybutynin, propiverine, solifenacin, tolterodine, and trospium chloride. Trials with intravesical antimuscarinic administration, drugs with less direct antimuscarinic effects , and drugs no longer used in clinical practice were excluded. In the case of multiple publications on the same patients, the most complete report was chosen for each trial.
Also Check: Chronic Bladder Infection In Men
Posterior Tibial Nerve Stimulation
Electrostimulation is included within the conservative therapies used to treat OAB by acting on the afferent nerves of the pelvic floor. When conducting a systematic review, two clinical trials compared the action of the electrostimulation with oxybutynin in patients with UUI, showing a similar efficacy between the two treatments .
Posterior tibial nerve stimulation is performed using a neuromodulator that utilizes the peroneal nerve for afferent access to the S3 spinal cord region. The mechanism that makes the neuromodulation of the bladderurethra reflexes possible is based on the fact that the nerve fibres of the posterior tibial region share sensitive inputs with the S3 root. Current indications include overactive bladder with or without UUI and chronic pelvic pain.
The stimulation can be done in a percutaneous manner with a thin 34 G needle inserted just below the medial malleolus of the ankle , although it can also be done in a transcutaneous manner . Adequate stimulation applied using the neuromodulator, regarding the frequency, intensity and length of the impulses, is demonstrated when the big toe is observed flexing or the remaining toes show extension or flexion. The normal treatment scheme consists of 12 weekly sessions of 30 min.
The side effects associated with this technique are infrequent and mild. The most common include cases of a painful feeling and transitory bleeding or bruising at the puncture site .
Antimuscarinic Drugs To Treat Overactive Bladder
- Accepted 20 January 2012
A 45 year old woman presents to her general practitioner complaining of troublesome urinary symptoms increasingly affecting her quality of life. She is currently voiding more than 10 times a day and rising three times at night. In addition she notices a sudden urgent desire to void and on two occasions has leaked urine before reaching the toilet. She gives no history of urinary tract infection or haematuria. Her periods remain regular.
In the past she has had two vaginal deliveries, has no significant medical history, and is not taking any medication. Pelvic examination is unremarkable and urine analysis normal. Ultrasound examination shows no post-void residual urine.
Based on the history, clinical examination, and basic investigations you make a symptomatic diagnosis of overactive bladder. After discussing her bladder symptoms, you offer lifestyle advice including the moderation of fluids and reduction of caffeine intake. In addition you refer her for bladder retraining and start treatment with antimuscarinic drugs.
Also Check: Surgical Treatment For Overactive Bladder
Read Also: Unable To Empty Bladder Female
Pelvic Floor Muscle Training
Two sessions of PFMT were applied to the patients in the treatment group for 12 weeks. Patients received 24 sessions in total. The patients could exercise comfortably in this exercise program. Patients with a PFM strength of 3 out of 5 or more were enrolled in the study. The PFM strength by digital palpation was done in the lithotomy position and graded , as on Oxford scale. A trial session was conducted before the first session to feel the pelvic floor muscles, to get used to the exercise, and to see the contraction. The therapy program duration was 40 min in total. Following the protocol of Ozlu at al. , the patients received a total of 80 treatment cycles with 10 s of contraction and 20 s of relaxation in each session. During the session, the contraction and relaxation of the pelvic floor muscles of the patients were displayed on the monitor to receive visual biofeedback. The contraction of the pelvic floor muscles was demonstrated with graphics or figures in front of the computer screen , and after verbal explanations, correct exercises were taught in the company of a pelvic physiotherapist. All patients in the study were trained by the same physiotherapist.
Prescription Drugs For Overactive Bladder
There are several prescription drugs for overactive bladder .
The FDA approved medications, or drugs, currently available on the U.S. market for the treatment of urinary incontinence are for a specific condition called overactive bladder . Some are also used for OAB with urge urinary incontinence . You may have seen advertisements on television or in magazines for these medications. Most of the prescription drugs for OAB partially calm the bladder muscles that cause abnormal contractions, thereby reducing the frequency and severity of the overwhelming urge to urinate. Some of these drugs may also increase the bladders capacity to hold urine and delay the initial urge to void. This class of drugs is referred to as antimuscarinics.
The currently FDA approved antimuscarinic drugs for OAB are: Oxybutynin, Tolterodine, Solifenacin, Hyoscyamine, and Darifenacin. These drugs are sold under the names of: Ditropan, Detrol, Vesicare, Enablex, Levbid, Cytospaz and Oxytrol. Most of these are oral medications and need a doctors prescription. Only one drug will be available over-the-counter as of September 2013, and it is in a skin patch form for women only.
Note: Drugs that are currently approved may be suddenly taken off the market, and new drugs are being introduced. Your healthcare provider and pharmacist can help you know which current drugs on the market may be the best for your circumstances.
Who May Need a Prescription?
Possible Side Effects
Also Check: How Long Can You Live With Stage 4 Bladder Cancer
Newer Agents For The Management Of Overactive Bladder
BENJAMIN J. EPSTEIN, PHARM.D., B.C.P.S., JOHN G. GUMS, PHARM.D., and EMERSON MOLINA, PHARM.D., University of Florida, Gainesville, Florida Fort Lauderdale, Florida
Am Fam Physician. 2006 Dec 15 74:2061-2068.
Overactive bladder is a clinical syndrome characterized by one or more symptoms of urgency , frequency , nocturia, and incontinence. In persons without overactive bladder, the need to empty the bladder becomes progressively more demanding in overactive bladder, urgency is characterized by unheralded messages of an immediate need to empty the bladder. These signals are difficult to delay. The inability to delay urination results in episodes of incontinence in up to 40 percent of patients with overactive bladder.
A = consistent, good-quality patient-oriented evidence B = inconsistent or limited-quality patient-oriented evidence C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, see page 2008 or.
Drug Therapy For Overactive Bladder
Home » Treatments » Drug therapy for overactive bladder
- Go to:
OAB symptoms are more common as people age, but they are not a normal part of ageing. They can be treated.
If you have bothersome symptoms, it is important that you go to your doctor. Try not to be embarrassed in discussing your situation. If self-management and lifestyle changes cannot control your symptoms, your doctor may suggest drug therapy. The goal is to reduce the urgent need to urinate and the number of times you need to go, as well as to prevent leakage episodes. Drugs used for OAB are antimuscarinic drugs or mirabegron . Together with your doctor, you can decide which type of drug treatment is best for you.
Factors which influence this decision include:
- Your symptoms
- Any other medication you are taking
- Drugs available in your country
- Your personal preferences and values
Recommended Reading: Muscle Invasive Bladder Cancer Survival
Rationale For Anticholinergic Use
Detrusor muscle contractions are essential for normal micturition, but involuntary contractions produce the symptoms of overactive bladder. Contractions depend on the activation of muscarinic receptors in the bladder by acetylcholine. The M3 muscarinic receptor-subtype is thought to be the most important in regulating detrusor contractions.
Anticholinergic drugs block muscarinic receptor activation and inhibit the spontaneous detrusor contractions found in overactive bladder. Drug efficacy is dose-dependent, but effectiveness is often limited by unwanted antimuscarinic effects in distant organs where other acetylcholine receptor-subtypes predominate . These adverse effects are also dose-dependent. They commonly include dry mouth, dry eyes, confusion, constipation, somnolence, blurred vision and increased heart rate.
There are no currently available drugs with pure selectivity for the muscarinic receptors in the detrusor. To try to improve the benefit:harm ratio a number of anticholinergics have been developed with greater selectivity for the detrusor or the M3 receptor, or with extended release properties.
A Mechanism Of Action And Pharmacological Properties:

Detrusor contractions are triggered mainly by acetylcholine -induced stimulation of muscarinic receptors on bladder smooth muscle :375-400.). ACh antagonists which bind to these receptors inhibit normal and involuntary detrusor contractions. Muscarinic receptors are also present in bladder urothelium and suburothelium, and there is a suggestion that Ach release by the urothelium and by suburothelial cholinergic fibers may influence detrusor function .
Of the five muscarinic receptor subtypes that have been identified in humans, the M2 is the predominant subtype, but M3 receptors mediate most bladder smooth muscle contraction :375-400., 2222. Giglio D, Tobin G. Muscarinic receptor subtypes in the lower urinary tract. Pharmacology. 2009 83:259-69.).
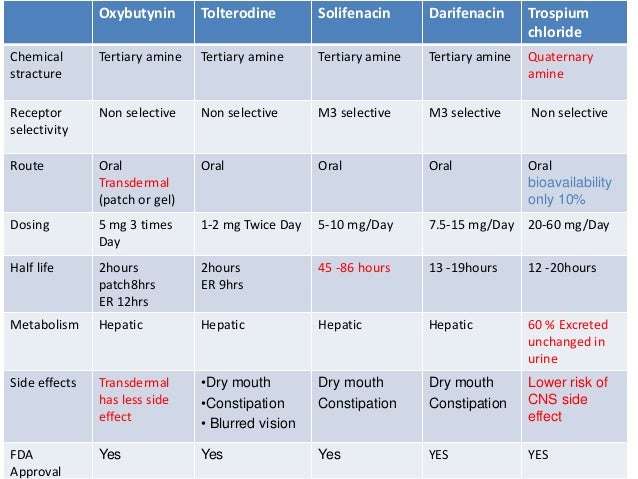
Antimuscarinic agents differ in molecular size, charge and lipophilicity. They are categorized as tertiary or quaternary amines. Tertiary agents have higher lipophilicity and less molecular charge, both of which along with small molecular size increase the passage through the blood-brain barrier . They include atropine, darifenacin, fesoterodine, oxybutynin, propiverine, solifenacin, and tolterodine. Quaternary agents such as propantheline and trospium have greater molecular charge and less lipophilicity with limited passage into the central nervous system and lower risk of CNS side effects .
Also Check: Azo Bladder Control & Weight Management
Pathophysiology Of The Oab Syndrome
Various factors may be involved in OAB and the major cause may vary from individual to individual. The etiology of OAB is still under investigation and is not well understood. However, 4 theories have been proposed to explain the pathophysiology of OAB:
The neurogenic theory: reduction in the inhibitory neural impulses and increase in the afferent impulses from the bladder trigger the voiding reflex .
The myogenic theory: the detrusor muscle becomes more sensitive to cholinergic stimulation leading to increased spontaneous activity .
The autonomous bladder theory: alteration or exacerbation of phasic activity is generated by muscarinic stimulation .
The afferent signaling theory: spontaneous bladder contractions during filling result in increased afferent output and hence the awareness of bladder filling .
D Adverse Effects And Contraindications:
Urinary retention and antimuscarinics: The inhibitory effect of antimuscarinics on detrusor contraction could worsen bladder emptying and contribute to urinary retention. Contrary to this hypothesis, the network meta-analytic study by Kessler et al. showed similar urinary tract related adverse events between antimuscarinics and placebo . The current understanding is such that the dose range used for beneficial effects in OAB is lower than that needed to produce a significant reduction in the voiding contraction . Consistent with this, the use of antimuscarinics in association with an alpha-blocker in men with BPH and a moderately enlarged prostate has been shown to be safe even in patients with a post-void residual of up to 150mL . Yet, monitoring PVR in patients with BPH and/or incomplete bladder emptying is recommended.
The use of antimuscarinics in high-risk individuals other than elderly subjects should also be avoided. Finally, the clinician should consider reconciling the medications of a given patient to reduce anticholinergic burden .
Also Check: How Do You Stop Bladder Leakage
Drug Therapy With Antimuscarinics
Antimuscarinics or Muscarinic receptor antagonists are a group of drugs which reduce the abnormal contractions of the bladder and improve urgency symptoms.
There are several MRAs. These work similarly, but they may have different side effects and be more or less tolerated by patients.
Taking antimuscarinics
Most antimuscarinics are taken by mouth once daily with or without food, although they can also be administered through a transdermal patch. The recommended dose for adults differs by the type of MRA. Start with the minimum dosage that gives you the beneficial effects of the drug with as few side effects as possible.
Antimuscarinics are not recommended for patients who are pregnant or those who suffer from conditions like:
- glaucoma
- severe constipation
Possible drug interactions
When antimuscarinics are taken by mouth, interactions with other drugs can occur. Ask your doctor about drug interactions. Read the prescription instructions for your drug treatment carefully to make sure you take medications correctly.
E Adherence And Persistence With Antimuscarinics:
Typically, adherence in clinical trials is much higher than in real world clinical practice . Studies from real world experience have reported average adherence periods of few weeks to few months with different antimuscarinics. Recent studies from Canada and the United Kingdom have confirmed low persistence rates for all the antimuscarinic agents. In the study from UK, the median time to discontinuation varied from 30 to 78 days . In the Canadian study, median time to discontinuation for the different antimuscarinics varied from 75 to 108 days, with around 20% of patients persisting on medication for 12 months .
Also Check: Does Azo Help With Bladder Infection
Side Effects Of Antimuscarinic Drugs And Safety Precautions
Dry mouth and constipation are the most common and bothersome side effects of antimuscarinic agents. In addition constipation may potentiate symptoms due to the effect of the presence of excessive stool in the rectal ampulla. This may decrease the bladder capacity and therefore, should constipation appear, an early use of fiber and stool softeners is recommended .
Constipation may lead to the discontinuation of medication in up to 50% of patients . Another reason for not following the recommended oral drug regime during the first 2 to 3 months may be that improvement appears gradually or only to a small degree.
Contraindications for the use of antimuscarinic agents are patients with closed angle glaucoma, myasthenia gravis, severe ulcerative colitis, a toxic megacolon, or intestinal obstruction because of their anticholinergic effects on the bowel. However, treatment decisions should be individualized and their prescription might need approval from the clinician caring for these disorders.
Compliance in using antimuscarinic may not be sufficient, as shown in a 2011 systematic review of 149 papers that found discontinuation rates of 4383% in the first 30 days of treatment, and more than half of patients never refilled the initial prescription . Regular follow-ups are important in monitoring treatment effects and adherence. All available antimuscarinic drugs come as an oral preparation.
Medicine For Stress Incontinence
If stress incontinence does not significantly improve with lifestyle changes or exercises, surgery will usually be recommended as the next step.
However, if you’re unsuitable for surgery or want to avoid an operation, you may benefit from an antidepressant medicine called duloxetine. This can help increase the muscle tone of the urethra, to help keep it closed.
You’ll need to take duloxetine tablets twice a day and will be assessed after 2 to 4 weeks to see if the medicine is beneficial or causing any side effects.
Possible side effects of duloxetine can include:
- nausea
- constipation
Do not suddenly stop taking duloxetine, as this can also cause unpleasant side effects. A GP will reduce your dose gradually.
Duloxetine is not suitable for everyone, however, so a GP will discuss any other medical conditions you have to determine if you can take it.
You May Like: Icd 10 Code For Urothelial Carcinoma Of Bladder