Mechanism Of Action For Pd
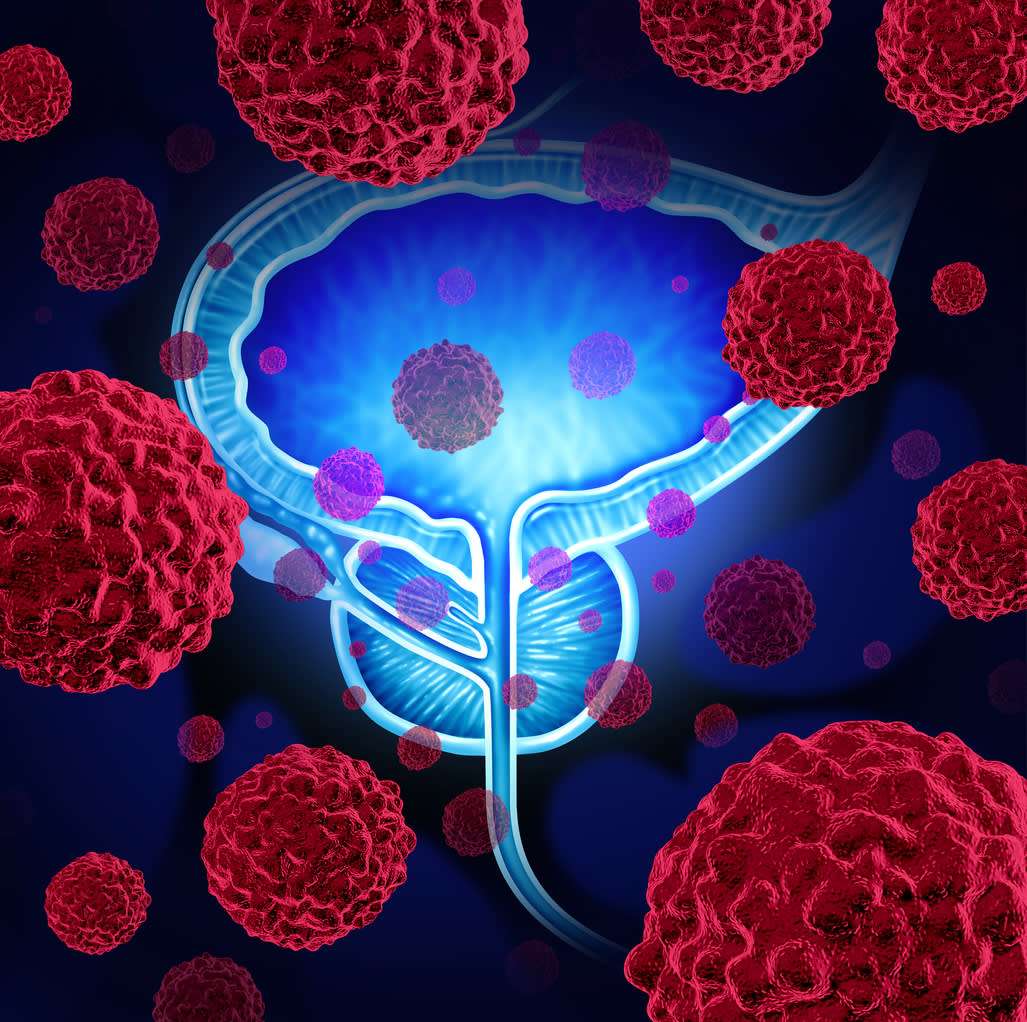
Figure 2 The cancer-immunity cycle in UBC. The cancer-immunity cycle is based on the illustration by Chen and Mellman . The cancer-immunity cycle can be divided into seven major steps, starting with the release of neoantigens from the cancer cells and ending with the killing of cancer cells . DC, dendritic cell.
The Mtor Kinase Inhibitors
The mammalian target of rapamycin kinase regulates many signaling pathways responsible for cell proliferation, angiogenesis, and growth. The mTOR inhibitors, such as everolimus or sirolimus, are used as immunosuppressive drugs .
Research on the use of these drugs to treat BC is ongoing. The drugs work by binding to the FKBP-12 protein, forming a complex that inhibits mTOR activity. This results in cell cycle arrest and the inhibition of angiogenesis, proliferation, and glucose delivery to cells . Angiogenesis is inhibited by the reduction in the expression of hypoxia-inducible factor 1, which in turn reduces the level of vascular endothelial growth factor .
In 2016, the FDA approved everolimus for adult patients with progressive neuroendocrine tumors of gastrointestinal or lung origin with unresectable, locally advanced, or metastatic disease . The efficacy of everolimus in BC treatment has been well documented both in vitro and in animal studies . A phase II trial involving patients with metastatic urothelial carcinoma revealed the antitumor activity of everolimus, albeit only in a subgroup of patients . In vitro studies have also shown the effectiveness of everolimus combined with cisplatin .
Who Can Have This Treatment
BCG is appropriate for noninvasive and minimally invasive bladder cancers. It usually follows a procedure called transurethral resection of bladder tumor . Its intended to help prevent recurrence.
This treatment only affects cells inside the bladder. Its not useful for later stage bladder cancer that has spread into or beyond the bladder lining, or to other tissues and organs.
Recommended Reading: How To Get Rid Of Bladder Leakage
Cystoscopy With Cautery Destruction Of The Bladder Tumor
Cystoscopy is an outpatient procedure during which a thin, lighted tube with a camera is passed through the urethra into the bladder, allowing your doctor to see the inside of the bladder.
Most modern cystoscopes are also equipped with channels that permit small instruments to be passed into the bladder. During a cystoscopy, your doctor may use these instruments to remove tissue, stop bleeding with a special electrical device called an electrocautery or even perform laser treatment. If the bladder cancer tumor is small enough, this cautery may be used to remove the cancer.
Is There A Role Of Bcg In Low Risk Bladder Cancer
Literature review and analysis
Low grade NMIBC that occur for the first time are considered low risk NMIBC. Although patients with low risk NMIBC have been shown in randomized studies to benefit from BCG in terms of risk reduction , its use must be weighed against the potential for side effects. In general, consensus guidelines do not recommend the use of BCG for these low risk tumors . The EAU and the AUA suggest consideration of the use of BCG when low grade tumors are large, multifocal, and/or recurrent . It has been noted that BCG can be less effective in low grade tumors, presumably because they are less antigenic .
Consensus recommendations
The Task Force unanimously recommended that low risk patients should not receive BCG .
Recommended Reading: Is Bladder Cancer Fast Or Slow Growing
Immunotherapy In The Neoadjuvant Setting
A phase II trial of neoadjuvant atezolizumab administration based on 1,200 mg for one, two, and three doses before cystectomy will give significant information regarding the effects of and requirement for multiple CPI applications . In this multi-dose portion trial, patients with adverse pathology at the time of cystectomy and no metastatic disease will be permitted to receive adjuvant atezolizumab for up to 16 cumulative doses. For NACT-ineligible patients, but fit to undergo surgical resection of their cancer by cystectomy, a combination phase II trial is underway comprising two nivolumab cycles, an antibody targeting PD-1 to reactivate T cells, plus urelumab, an CD137-agonistic antibody with additional activating properties, will be compared to two cycles of nivolumab alone . In addition, a pilot presurgical study will evaluate durvalumab and tremelimumab safety for this, 28 patients are enrolled. This will determine if this is an effective and safe neoadjuvant therapy for MIBC patients who are not eligible for cisplatin-based therapy .
If Your Immunotherapy Stops Working
Immunotherapy may not work for everyone who takes it. If youâve tried it and it didnât stop your cancer, you still have a few options. What kind of treatment you get next depends on what others youâve tried and what stage your cancer is in.
This treatment uses powerful drugs to kill cancer. Even if youâve already tried some drugs before or along with your immunotherapy, your doctor may try other ones or different combinations of medicines to fight your cancer. Chemo drugs for the most common form of bladder cancer include:
Youâll get chemotherapy in cycles with a few weeks in between to give your body time to recover.
Surgery
If you still have all or part of your bladder, your doctor might recommend an operation called a radical cystectomy. Your doctor will take out all of your bladder and the lymph nodes nearby. They might also remove some of your reproductive organs. For men, that could be the prostate gland and seminal vesicles. For women, it might be the ovaries, fallopian tubes, uterus, cervix, and a small part of the vagina.
If you think you might want to join a clinical trial, your doctor will help you make the decision. They will talk about:
- How the new treatment is different from the usual treatments you could get
- What the risks are
- Any tests youâll need
- How often youâll get treatment
Youâll be able to leave the clinical trial whenever you want, for whatever reason you might have.
You May Like: What Can You Do For An Overactive Bladder
Bladder Cancer Consensus Task Force
The Task Force consisted of 17 participants, including 8 medical oncologists, 7 urologists, 1 nurse, and 1 patient representative . The urologists were chosen for their experience in the development and evaluation of best practice guidelines for the use and optimization of BCG therapy, and all members were experts in the management of the spectrum of urothelial cancer. The medical oncologists were experienced in the management of advanced bladder cancer with both chemotherapy and immunological therapy, including participation in clinical trials of immune checkpoint inhibitors. Additional participants were experts in addressing issues of barriers in access to appropriate use of immunotherapy. A list of the Task Force pre-meeting survey questions and responses is available in Additional file .
Perioperative Immunotherapy In Muscle
Hyung Ho Lee1, Won Sik Ham2
1 Department of Urology, Urological Science Institute , Yonsei University College of Medicine , , Korea
Contributions: Conception and design: WS Ham Administrative support: WS Ham Provision of study materials or patients: WS Ham Collection and assembly of data: All authors Data analysis and interpretation: All authors Manuscript writing: All authors Final approval of manuscript: All authors.
Correspondence to:
Keywords: Chemotherapy muscle-invasive bladder cancer immune checkpoint inhibitors programmed death-receptor 1 programmed death-receptor ligand 1
Submitted Nov 23, 2019. Accepted for publication Jan 08, 2020.
doi: 10.21037/tcr.2020.01.36
Recommended Reading: How Does Bcg Work For Bladder Cancer
What Is The Optimal Timing And Schedule Of Post
Literature review and analysis
Most guidelines recommend intravesical immunotherapy be initiated after an interval of at least two weeks following transurethral resection or biopsy of the bladder to avoid systemic absorption , unless repeat resection is to be performed . Unlike chemotherapy, BCG should never be administered within 24 h of bladder tumor resection and can in fact be dangerous. Non-randomized studies show no advantage of early administration. There are no randomized data suggesting an optimal time to first dose . Additionally, patients who tolerate 6 weeks of BCG induction and are at high risk for tumor recurrence and progression should be treated with maintenance BCG using the SWOG schedule: 3 weekly instillations at 3, 6, 12, 18, 24, 30, and 36 months .
Consensus recommendations
The Task Force agreed with the recommendation to wait at least 2 weeks before instillation of BCG after resection of tumor based on Level A evidence. In addition, the Task Force agrees with the 6 + 3 schedule of maintenance BCG administration based on Level A Evidence.
Intermediate Risk Early Bladder Cancer
People with intermediate-risk non-muscle-invasive bladder cancer should be offered a course of at least 6 doses of chemotherapy. The liquid is placed directly into your bladder, using a catheter, and kept there for around an hour before being drained away.
You should be offered follow-up appointments at 3, 9 and 18 months, then once every year. At these appointments, your bladder will be checked using a cystoscopy. If your cancer returns within 5 years, you’ll be referred back to a specialist urology team.
Some of the chemotherapy medicine may be left in your urine after treatment, which could severely irritate your skin.
It helps if you sit down to urinate and that you’re careful not to splash yourself or the toilet seat. Always wash the skin around your genitals with soap and water afterwards.
If you’re sexually active, it’s important to use a barrier method of contraception, such as a condom. This is because the medicines may be present in your semen or vaginal fluids, which can cause irritation.
You also shouldn’t try to get pregnant or father a child while having chemotherapy for bladder cancer, as the medicines can increase the risk of having a child with birth defects.
Don’t Miss: Does D Mannose Help Overactive Bladder
What Happens During Treatment
A urinary catheter is inserted through your urethra and into your bladder. Then the BCG solution is injected into the catheter. The catheter is clamped off so the solution stays in your bladder. Some doctors may remove the catheter at this time.
You have to hold the medicine in your bladder. Youll be instructed to lie on your back and to roll from side to side to make sure the solution reaches your entire bladder.
After about two hours, the catheter is unclamped so the fluid can be drained. If the catheter was already removed, youll be asked to empty your bladder at this time.
Consensus Panel And Conflicts Of Interest
In accordance with the practices utilized in previous SITC consensus guidelines, panel members were both SITC members or nonmembers but represented multiple disciplines, including patient representatives, nurses, and others expected to be affected by the development of clinical practice guidelines. All Task Force members were required to disclose any conflicts of interest using the SITC disclosure form, which requires full financial and other disclosures concerning relationship with commercial entities that could be expected to have direct regulatory or commercial impact resulting from the publication of this statement. An advanced copy of this manuscript was available for comment by SITC membership prior to publication . No commercial funding was provided to support the consensus panel, literature review, or the preparation of this manuscript.
Don’t Miss: How Long Can You Live With Aggressive Bladder Cancer
Catheterizable Continent Diversion Pouch
This is a reservoir of bowel with a stoma that is catheterizable for emptying the bladder. The urine is siphoned out of the urinary reservoir with a small catheter every four to six hours. The catheterizable pouch may require surgical repair at some point after surgery due to the wear and tear of frequent catheterization. This type of reconstruction is not performed on patients with a history of bowel disease.
What Is The Role Of Bcg In Intermediate Risk Bladder Cancer
Literature review and analysis
Consensus recommendations
The Task Force discussed risk stratification at length and agreed that there were varying definitions of intermediate risk. However, most felt that that most of these patients would benefit from BCG based on Level A evidence from randomized clinical trials. The Task Force unanimously advocated for risk stratification as a basis for deciding therapy and recommend that the risk category for the tumors be carefully assessed and the transition from low risk to intermediate risk be carefully defined. The EORTC 30911 study comparing 3-week maintenance BCG and epirubicin chemotherapy found that intermediate risk patients had even a greater reduction in metastasis and mortality than high risk patients . Thus, the Task Force recommends that BCG induction and at least 1 year of maintenance therapy be used for patients with intermediate risk tumors.
Read Also: Does Drinking Water Help With Overactive Bladder
Intravesical Therapy For Bladder Cancer
With intravesical therapy, the doctor puts a liquid drug right into your bladder rather than giving it by mouth or injecting it into your blood. The drug is put in through a soft catheter that’s put into your bladder through your urethra. The drug stays in your bladder for up to 2 hours. This way, the drug can affect the cells lining the inside of your bladder without having major effects on other parts of your body.
Substantial Improvement In Survival
Dr. Powles and his colleagues enrolled 700 people with locally advanced or metastatic bladder cancer in the international JAVELIN Bladder 100 study, which was funded by Pfizer, the drug’s manufacturer.
All trial participants had already received chemotherapywith either cisplatin and gemcitabine or carboplatin and gemcitabine, if their health did not allow them to receive cisplatinand their disease had not worsened during chemotherapy.
Participants were then randomly assigned to receive either maintenance treatment with avelumab plus supportive care or supportive care alone. People in the maintenance group received infusions of avelumab every 2 weeks until their cancer started growing again or they left the study for other reasons. Supportive care for both groups included pain management, nutritional support, and treatment of infections.
People in the supportive care group whose cancer got worse did not receive avelumab as part of the trial. However, they could receive it or any other immunotherapy drug after leaving the study.
Maintenance treatment with avelumab after chemotherapy turned out to have substantial benefits. The median overall survival for people who received maintenance avelumab was more than 21 months, compared with about 14 months for people who received only supportive care until their cancer got worse.
Don’t Miss: I Have A Weak Bladder Help
Checkpoint Inhibitor Drugs For Bladder Cancer
Checkpoint inhibitor drugs release a natural brake on the immune system. This allows the immune cells called T cells to recognize and attack tumors. The drugs work by blocking the interaction of a molecule called PD-1 on the surface of immune cells with a molecule called PD-L1 on the surface of cancer cells.
Since 2016, four checkpoint inhibitor drugs have become available for the treatment of bladder cancer:
Who Can Use Bcg
BCG is a treatment for early-stage bladder cancer that has not yet invaded the muscle of the bladder wall. Called non-muscle invasive bladder cancers or in situ bladder cancers, these account for about half of all bladder cancers.
For 2021, it was estimated that about 83,730 new cases of bladder cancer would be diagnosed in the United States, and about 17,200 American bladder cancer patients would die from the disease.
Don’t Miss: Side Effects Of Bladder Cancer Chemotherapy
Neoadjuvant Chemotherapy In Mibc
Several randomized controlled trials and meta-analyses have investigated the contribution of NACT, administered before radical cystectomy, to improving survival. One meta-analysis reported that cisplatin-based combination NACT can result in a 16% reduction in overall risk of death, compared to that with locoregional therapy alone. When considering only regimens comprising cisplatin/carboplatin or methotrexate, vinblastine, doxorubicin, and cisplatin -like chemotherapy, NACT is related to even better survival with an absolute 5-year survival benefit of 8% . In these studies, PBCT was used, and the results are not suitable for supporting non-cisplatin-based therapy in the neoadjuvant environment. Some adjuvant studies also showed similar efficacy with a gemcitabine-cisplatin combination, which is less toxic and has been expanded to a neoadjuvant setting .
Moffitts Approach To Bladder Cancer Immunotherapy
Moffitt Cancer Center believes in taking a multispecialty approach to the treatment of cancer. The bladder cancer team within our Urologic Oncology Program comprises experts in all specialties, including chemotherapy, radiation therapy, surgery, immunotherapy and more. This ensures that all angles of treatment are considered and that a patients individualized treatment plan includes the most appropriate therapies for the best possible outcome and quality of life.
Moffitt is recognized for its groundbreaking research and robust clinical trials program, which includes a range of immunotherapy options for treating bladder cancer. Due to these research efforts alongside our comprehensive treatment and supportive care, we have been recognized as a Comprehensive Cancer Center by the National Cancer Institute the only cancer center based in Florida to hold this designation.
For more information about bladder cancer immunotherapy, or to consult with oncologists specializing in the treatment of bladder cancer, call Moffitt at or complete a new patient registration form online.
- BROWSE
You May Like: How Do Poise Bladder Supports Work
Other Treatments For Bladder Cancer
For many early-stage bladder cancers, BCG is the best option for treatment. Other treatments for bladder cancer include:
- Surgery to remove the tumor: Early cancers can be removed with TURBT surgery. More advanced cancers may require more extensive surgery, like removal of part or all of the bladder .
- Intravesical chemotherapy: This treats the inside of the bladder with chemotherapy drugs. Chemotherapy drugs commonly used for bladder cancer include Mutamycin , Gemzar , or Valstar .
- Radiation therapy
- Clinical trials
Subtleties And Future Questions
Several factors have to be carefully considered in interpreting the trial results, explained Dr. Apolo.
A major one is that the study did not directly compare survival between people who got avelumab immediately versus when their cancer progressed. Only about half of the participants who initially received supportive care alone went on to receive immunotherapy after their cancer got worse. There could be many reasons for this, including lack of access to these drugs in different countries, Dr. Apolo said.
But it also might be that, for some people, the cancer was progressing too rapidly, she added. When these tumors start growing, they start growing very quickly. So if you wait to start at the time of progression, maybe its too late, added Dr. Apolo.
Not all patients will be caught by the second-line safety net, agreed Dr. Plimack.
So, for now, said Dr. Balar, the takeaway message from the JAVELIN study is after chemotherapy, dont wait to give immunotherapy.
But more and more, studies are looking at whether some patients should receive immunotherapy as first-line treatment, he continued. Immunotherapy is one of the most important advances weve made in the last 30 years, Dr. Balar said.
The JAVELIN results cant provide any insight into which patients benefit from first-line treatment with a platinum-based chemotherapy, he added. This trial wasnt designed to ask: Is chemotherapy necessarily the best choice for every patient? he explained.
Don’t Miss: Bladder Cancer What To Expect