What Is Bladder Cancer
Bladder cancer starts when cells that make up the urinary bladder start to grow out of control. As more cancer cells develop, they can form a tumor and, with time, spread to other parts of the body.
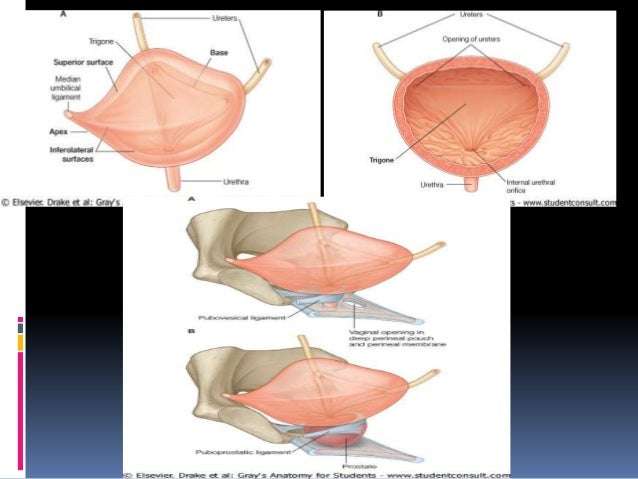
The bladder is a hollow organ in the lower pelvis. It has flexible, muscular walls that can stretch to hold urine and squeeze to send it out of the body. The bladderâs main job is to store urine. Urine is liquid waste made by the 2 kidneys and then carried to the bladder through 2 tubes called ureters. When you urinate, the muscles in the bladder contract, and urine is forced out of the bladder through a tube called the urethra.
The Icd Code C67 Is Used To Code Bladder Cancer
Bladder cancer is any of several types of cancer arising from the epithelial lining of the urinary bladder. Rarely the bladder is involved by non-epithelial cancers, such as lymphoma or sarcoma, but these are not ordinarily included in the colloquial term âbladder cancer.â It is a disease in which abnormal cells multiply without control in the bladder.
| Specialty: |
- DRG Group #656-661 â Kidney and ureter procedures for neoplasm with MCC.
- DRG Group #656-661 â Kidney and ureter procedures for neoplasm with CC.
- DRG Group #656-661 â Kidney and ureter procedures for neoplasm without CC or MCC.
- DRG Group #656-661 â Kidney and ureter procedures for non-neoplasm with MCC.
- DRG Group #656-661 â Kidney and ureter procedures for non-neoplasm with CC.
- DRG Group #656-661 â Kidney and ureter procedures for non-neoplasm without CC or MCC.
- DRG Group #686-688 â Kidney and urinary tract neoplasms with MCC.
- DRG Group #686-688 â Kidney and urinary tract neoplasms with CC.
- DRG Group #686-688 â Kidney and urinary tract neoplasms without CC or MCC.
A Quick Guide To Bladder Cancer Icd 10 You Should Know
by Adam Smith | Jul 26, 2021 | Fitness, Healthy Lifestyle |
Want to know about bladder cancer icd 10? If there is a growth of abnormal tissues called tumors in the bladder lining of a person. Or it is spreading into the bladder muscle it is called bladder cancer. Do you know that thousands of men and women face this deadly disease every year around the world?
The ICD-10-CM which stands for International Classification of Diseases, Tenth Revision, Clinical Modification is a system. Healthyell providers and physicians use it to classify and code the symptoms, diagnoses, and procedures that are recorded in conjunction with hospital care in the United States.
Read Also: Surgical Treatment For Overactive Bladder
How A Lung Neoplasm Is Diagnosed
If you have ongoing respiratory symptoms that suggest a lung neoplasm, your healthcare provider may start by taking a detailed medical history.
Your healthcare provider will perform a focused physical exam, listening to the heart and lungs for sounds like wheezing and crackling that may be concerning for associated lung-related diseases, like COPD and emphysema, which increase ones chances of malignancy.
Imaging is usually ordered next. The following tests are initially performed to help provide more details on the lung neoplasm:
- Chest X-ray: This test is usually the quickest and least expensive imaging test, so it is used first. It is a painless scan that can show tumors 1 centimeter wide or larger.
- CT scan: CT scans use low-radiation X-ray beams to take many pictures of the inside of your body. They can help detect smaller lung cancers and provide more details than an X-ray.
- Lung function test : Also known as spirometry, this test measures how much air the lungs can hold and how quickly the lungs can be filled with air and then emptied.
- Blood tests. A sample of your blood may be tested to check the number of red blood cells, white blood cells, and platelets , and to see how well your kidneys and liver are working. Because lung cancer can throw off these numbers, comparing your baseline numbers to your current numbers can help provide details on potential changes that have occurred as a result of your lung cancer.
Causes Of Lung Neoplasms
Smoking in any form, including traditional cigarettes, hookah, snuff, cigars, and pipe tobacco, is the single biggest risk factor for lung neoplasms. The 60 or so carcinogens, or cancer-causing chemicals, in tobacco smoke account for more than 80%90% of lung cancer cases.
Research shows that smokers are 1530 times more likely to get lung cancer or die from lung cancer than nonsmokers. Your risk of developing lung cancer increases proportionally with the number of cigarettes you smoke in your lifetime.
Smoking isnt the only cause of lung neoplasms. Benign lung neoplasms can develop from an abscess, inflamed tissue, or cysts or as a result of scarring from an infection or pneumonia. Other causes of lung neoplasms are:
- A history of radiation therapy
- Exposure to asbestos, radon gas, or other carcinogens like heavy metals and diesel exhaust
- Exposure to industrial chemicals in the workplace, such as arsenic, nickel, silica, and chromium
- Genetic alterations and hereditary conditions
- Secondhand smoke exposure
- Air pollution
Sometimes, genetics may predispose you to lung cancer. This is more likely the case in individuals with an immediate nonsmoking family member who has or had lung cancer.
Familial forms of lung cancer may be influenced by several nongenetic factors, including similar lifestyles, such as diet and exercise, and similar environments, like living in areas with high levels of indoor and outdoor air pollution.
Recommended Reading: What Are The Best Pads For Bladder Leakage
Other Types Of Bladder Cancer
Approximately 2% of bladder cancers are adenocarcinomas. Nonurothelial primary bladder tumors are extremely rare and may include small cell carcinoma, carcinosarcoma, primary lymphoma, and sarcoma . Small cell carcinoma of the urinary bladder accounts for only 0.3-0.7% of all bladder tumors. High-grade urothelial carcinomas can also show divergent histologic differentiation, such as squamous, glandular, neuroendocrine, and sarcomatous features.
Malignant Neoplasm Of Overlapping Sites Of Bladder
- 2016201720182019202020212022Billable/Specific Code
- C67.8 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes.
- The 2022 edition of ICD-10-CM C67.8 became effective on October 1, 2021.
- This is the American ICD-10-CM version of C67.8 â other international versions of ICD-10 C67.8 may differ.
- Applicable To annotations, or
You May Like: Antibiotics Given For Bladder Infection
Don’t Miss: Can A Prolapsed Bladder Cause Lower Back Pain
Bladder Cancer Clinical Trials
What about Clinical Trials?
You may hear about clinical trials for your bladder cancer. Clinical trials are research studies that test if a new treatment or procedure is safe and effective.
Through clinical trials, doctors find new ways to improve treatments and the quality of life for people with disease. Trials are available for all stages of cancer. The results of a clinical trial can make a major difference to patients and their families. Please visit our clinical trials research webpage to learn more.
What Is A C67 Neoplasm Of The Bladder
Malignant neoplasm of bladder C67- > . A primary or metastatic malignant neoplasm involving the bladder. The bladder is a hollow organ in your lower abdomen that stores urine. Bladder cancer occurs in the lining of the bladder. People with a family history of bladder cancer or who are older, white, or male have a higher risk.treatments
Also Check: How To Reduce Bladder Inflammation Naturally
You May Like: Heavy Feeling In Bladder And Frequent Urination
Types Of Lung Neoplasms
Benign lung neoplasms are noncancerous and are usually classified by the tissues from which they arise. Benign lung neoplasms include:
- Hamartomas: Hamartomas are the most common type of benign lung nodule, accounting for about 55% of all benign lung tumors. They are unique in that these tumors consist of a variety of cell types, including muscle, fat, and cartilage. They are most often found on the periphery of the lung, along the outer edges. These coin-shaped tumors are usually small in size, oftentimes measuring 4 centimeters or less in diameter, and are commonly found accidentally on an X-ray.
- Bronchial adenomas: These neoplasms arise from the mucus glands or ducts of your windpipe or the large airways of the lungs. They are slow growing and rarely become malignant. Some types of bronchial adenomas are more common than others. For example, carcinoids account for 85% of bronchial adenomas .
- Papillomas: Arising from salivary glands, these are the least common type of benign lung neoplasm. They usually grow in the bronchial tubes. The two most common types of papillomas are squamous and glandular. Squamous papillomas are the result of the human papilloma virus . The cause of glandular papillomas remains a mystery.
Malignant lung neoplasms are cancerous and include three main types:
Other lung tumors that may affect the lungs include lymphomas, adenoid cystic carcinomas, and sarcomas. These types of cancer are treated differently than the more common lung cancers.
Prognosis In Squamous Cell Carcinoma
Tumor stage, lymph node involvement, and tumor grade have been shown to be of independent prognostic value in SCC. However, pathologic stage is the most important prognostic factor. In one relatively large series of 154 cases, the overall 5-year survival rate was 56% for pT1 and 68% for pT2 tumors. However, the 5-year survival rate for pT3 and pT4 tumors was only 19%.
Several studies have demonstrated grading to be a significant morphologic parameter in SCC. In one series, 5-year survival rates for grade 1, 2, and 3 SCC was 62%, 52%, and 35%, respectively. In the same study of patients undergoing cystectomy, the investigators suggested that a higher number of newly formed blood vessels predicts unfavorable disease outcome.
In SCC, the survival rate appears to be better with radical surgery than with radiation therapy and/or chemotherapy. In locally advanced tumors, however, neoadjuvant radiation improves the outcome. Sex and age have not been prognostically significant in SCC.
You May Like: Best Home Remedy For Bladder Infection
What Is The Icd 10 Code For Neoplasm
C67.9 is a billable/specific ICD-10-CM code that can be used to indicate a diagnosis for reimbursement purposes. The 2021 edition of ICD-10-CM C67.9 became effective on October 1, 2020. This is the American ICD-10-CM version of C67.9 other international versions of ICD-10 C67.9 may differ. All neoplasms are classified in this chapter, whether
Also Check: Bladder Problems After Gastric Bypass
What Is A Bladder Neoplasm

A bladder neoplasm is a tumor which develops in the bladder. Although it is an abnormal growth, a bladder neoplasm is not always cancer. Neoplasia, or new growth, can also take the form of a benign tumor, which is not cancerous. In the bladder, benign tumors are found less often than malignant tumors. A malignant tumor usually arises from the lining of the bladder, known as the urothelium.
Benign bladder tumors are quite rare. The two main types of benign neoplasm are known as transitional cell papilloma and nephrogenic adenoma. Sometimes a benign tumor may not cause any symptoms and it could be discovered during an investigation for another condition. In other cases, patients may discover blood in their urine. There is not usually any pain associated with this.
Malignant neoplasms are relatively common. Worldwide, the most frequently occurring type of bladder cancer is known as squamous cell carcinoma. In developed countries, a type of cancer called transitional cell carcinoma is more commonly found. The symptoms associated with bladder malignancy are similar to those experienced with benign tumors. Blood is seen in the urine, but there is not any pain, as there would be with other disorders such as a urinary tract infection.
Read Also: What Causes Chronic Bladder Infections
Therapy: Treatment Options For Cancer Vary
Treatment options depend on the stage of the cancer and may include surgery, chemotherapy, or radiation.
Surgery may involve removing a small tumor or polyp only, or removing a tumor and a portion of the surrounding tissue, if the tumor is larger or has spread into nearby tissue. The surgeon may also remove some lymph nodes near the area of cancer if its known the cancer has spread to them, or to see if the cancer has spread to them.
Chemotherapy drug therapy may be used before surgery to shrink the size of tumors, or after surgery to kill any remaining cancer cells that may have spread to other parts of the body.
Radiation therapy may similarly be given to shrink tumors before surgery or to kill any remaining cancer cells after surgery. It may also be used in place of surgery in some cases.
How To Prevent Bladder Cancer
The study on bladder cancer is still going on. Moreover, the doctors do not know its causes so you can try out some of the common preventing ideas by professionals. You should avoid smoking as it can kill immunity and decreases the life of a person. Also, you should drink plenty of water every day so the system of your body works properly.
If you feel the symptoms of even slight pain, you should never take it lightly. Bladder cancer can be deadly for you and it can spread quickly if not taken care of.
Read Also: How To Stop An Overactive Bladder At Night
Bladder Cancer Icd 10 Types Of Bladder Cancer:
After the diagnosis of the tumor, bladder cancer classifies based on how much it has spread. Here are the types of bladder cancer that can happen:
- Non-muscle invasive bladder cancer:
If the tumor cells have not spread outside the lining of the bladder, it is non-muscle-invasive bladder cancer. It is the most common type of bladder that does not cause death.
- Muscle invasive bladder cancer:
When the tumor cells spread outside the lining, and affect the bladder muscle, it is muscle-invasive bladder cancer. This type is rare but the chances of death are more.
- Metastatic bladder cancer:
If bladder cancer has not only spread to the bladder muscle but also other parts of the body, it is called metastatic bladder cancer.
Comparisons Of Os And Css For Patients In Different Risk Stratification Systems
To determine the independent discrimination of the novel prognostic nomogram, the low- and high-risk stratification systems for OS and CSS were constructed according to the total risk scores of the established nomogram . The cohort was divided into the low-risk , and high-risk groups for OS, and into the low-risk , and high-risk groups for CSS. Furthermore, the logrank test and KaplanMeier curves were further applied to determine the OS and CSS of MIBC patients in different prognostic risk stratification systems, the prognostic nomogram could discriminate MIBC patients with different risk stratification systems . Group adjuvant chemotherapy showed significantly better OS and CSS than group non-adjuvant chemotherapy before risk stratification . Furthermore, the different risk stratification subgroups showed that adjuvant chemotherapy had better OS and CSS than without adjuvant chemotherapy for high-risk patients while the OS and CSS for low-risk patients were comparable .
Don’t Miss: Uncontrollable Bladder After Giving Birth
Genetic Factors In Pathogenesis
Divergent, yet interconnected and overlapping, molecular pathways are likely responsible for the development of noninvasive and invasive bladder tumors. Somatic mutations in fibroblast growth receptor3 and tumor protein p53 in tumor cells appear to be important early molecular events in the noninvasive and invasive pathways, respectively.
FGFR-3, Ras, and PIK3CA mutations occur with high frequency in noninvasive tumors, leading to upregulation of Akt and mitogen-activated protein kinase . Loss of heterozygosity on chromosome 9 is among the most frequent genetic alterations in bladder tumors and is considered an early event.
Large numbers of genomic changes have been detected using karyotyping and comparative genomic hybridization analysis in urothelial carcinoma. Numerically common are losses of 2q, 5q, 8p, 9p, 10q, 18q, and Y. Gains of 1q, 5p, 8q, and 17q are frequently present, and high-level amplifications can be found however, the target genes in the regions of amplifications have not been conclusively identified.
Alterations in the TP53 gene are noted in approximately 60% of invasive bladder cancers. Progression-free survival is significantly shorter in patients with TP53 mutations and is an independent predictor of death among patients with muscle-invasive bladder cancer.
Pathology: Examining Tissue For Signs Of Cancer
When a polyp or other area of suspicious tissue is seen during a cancer screening test, the doctor may take a tissue sample called a biopsy right away, depending on the bodily location being examined, or at a later date, if doing so requires a second procedure. A pathologist then examines the tissue under a microscope to look for cancerous cells.
To better visualize the various parts of the tissue, the pathologist often stains it, sometimes with multiple dyes.
The pathologist looks for abnormalities in the shape and size of cells, shape and size of cell nuclei, and distribution of the cells in the tissue, indicating cancer.
Once the pathologist has confirmed that a biopsy shows cancer, other lab tests may be done to help classify the cancer, which can in turn help to guide treatment.
While much of the work of examining tissue samples is still done by individuals looking through microscopes, advances in automated detection and classification of cancer cells promise faster diagnosis and treatment.
Recommended Reading: Difference Uti And Bladder Infection
Risk Groups For Early Bladder Cancer
Doctors put early bladder cancer into 3 risk groups. These groups describe how likely it is that your cancer will spread further, or come back after treatment.
The 3 risk groups are:
- low risk
- intermediate risk
- high risk
Your doctor tells you whether your cancer is low risk, intermediate risk or high risk. Knowing your risk group helps them decide which tests and treatment are best for you.
Your risk group depends on:
- the size of your tumour
- what the cells look like under a microscope
- how many tumours there are
- the type of bladder tumour
- whether you have had treatment in the last year for early bladder cancer