Increases Risk Of Bladder Cancer
According to the American Cancer Society, a lack of fluids is considered a risk factor for bladder cancer. Flushing the bladder with hydrating liquids, especially water, means you urinate more often and keep cancer-causing chemicals from sitting in your bladder too long.
Also, keep a check on your urine color to be sure its not too concentrated. Chances are, plenty of nasty chemicals live in that high volume of waste, and you dont want that hanging around in your bladder!
Donât Miss: Tb Virus Treatment For Bladder Cancer
Which Bacteria Cause Uti
Escherichia coli is the most common cause of UTI and is responsible for about 80 to 85% of all UTIs. Other bacteria involved in UTIs include Staphylococcus saprophyticus, Klebsiella, Pseudomonas and Enterococcus. UTIs are rarely due to viral, fungal and parasitic infections.
You May Like: Can Bladder Cancer Be Seen On Ultrasound
Four Common Causes Of Hematuria
Written by Sarah Thebarge, Physician Assistant
Hematuria is a condition in which red blood cells are found in the urine. Hematuria can be macroscopic , where blood is visible with the naked eye, or it can be microscopic, only visible when examined under a microscope.
Here are four of the most common causes of this condition.
Recommended Reading: Is Bladder Infection Same As Urinary Tract Infection
When Is Surgery Needed For A Prolapsed Bladder
Severe prolapsed bladders that cannot be managed with a pessary and/or behavioral therapy usually require surgery to correct them. There are several different types of surgery depending on the severity of the prolapse and whether or not other organs are affected.
- The bladder is repaired with an incision in the vaginal wall.
- The prolapsed area is closed and the wall is strengthened. This may be done primarily using one’s own tissues or through the use of grafts, which may be biologic or synthetic .
- If one has stress urinary incontinence, this is also corrected.
- Depending on the procedure, surgery can be performed while the woman is under general, regional, or local anesthesia. Most women are discharged home on the same day of surgery.
- Various materials have been used to strengthen pelvic weakness associated with prolapsed bladder. A surgeon should explain in detail the risks, benefits, and potential complications of these materials, and he or she should explain the procedure itself before proceeding with the surgery. Complications related to surgery may include bleeding, infection, pain, urinary incontinence, recurrent prolapse, trouble urinating, and injury to the bladder.
- The cost of surgical treatment will vary with the procedure performed, the length of hospitalization, and the presence/absence of other medical conditions.
- After surgery, most women can expect to return to a normal level of activity after 6 weeks.
Addition Information About Vaginal Surgery When A Synthetic Or Biologic Graft Is Used
In Australia, in January 2018 the TGA withdrew approval for the used of synthetic and biologic mesh for trans-vaginal prolapse repair. The TGA continues to approve synthetic and biological mesh for prolapse when placed using laparoscopy, robot assisted and through an abdominal incision.
In the USA, the Food and Drug Administration has issued the following safety communication regarding the use of mesh.
The FDA wants to inform you about the complications that can occur when surgical mesh is used to treat Pelvic Organ Prolapse and Stress Urinary Incontinence , and provide you with questions to ask your surgeon before having these procedures. This is part of our commitment to keep healthcare professionals and the public informed about the medical products we regulate.
Background
Pelvic organ prolapse can cause pain or problems with bowel and bladder functions or interfere with sexual activity.
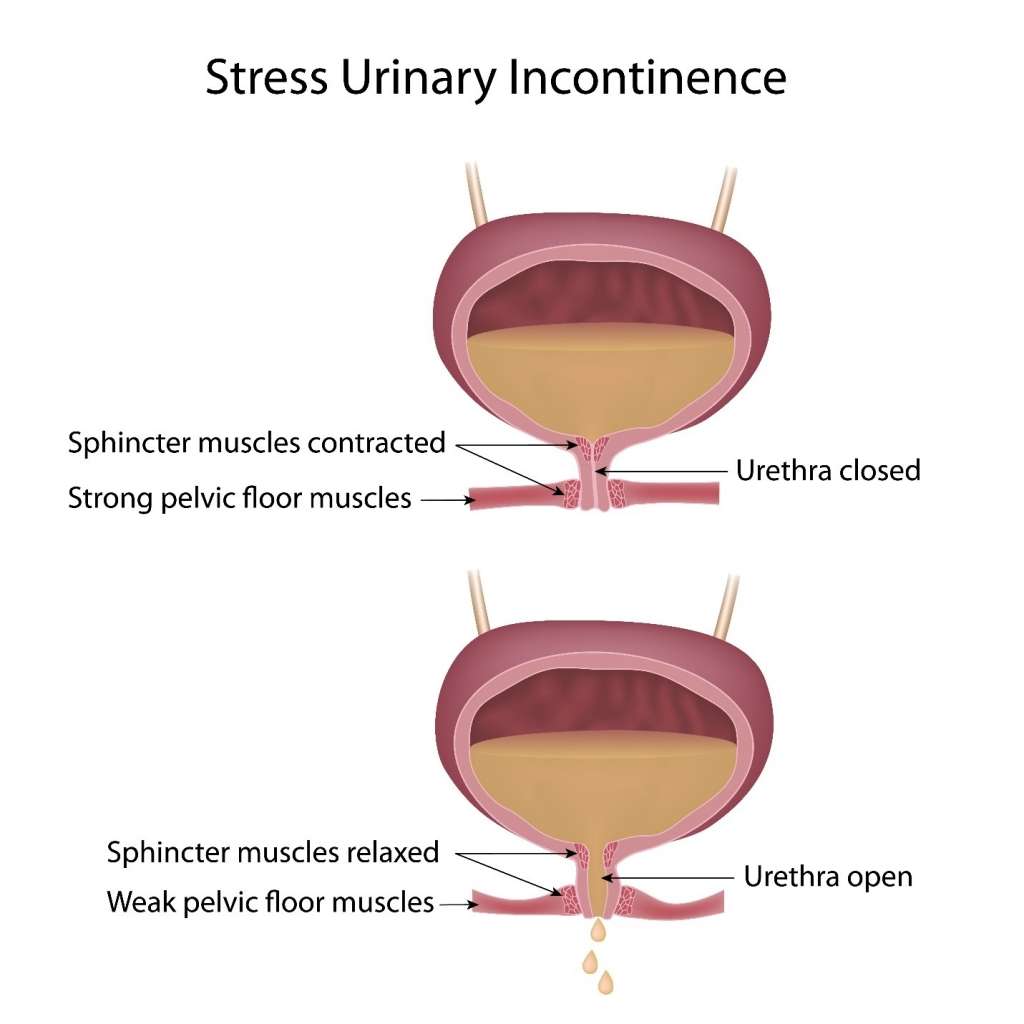
Stress urinary incontinence is a type of incontinence caused by leakage of urine during moments of physical stress.
Talking to your doctor
Before having an operation for POP or SUI, be sure to let your surgeon know if youve had a past reaction to mesh materials such as polypropylene.
Questions you should ask the surgeon before you agree to surgery in which mesh will be used:
Read Also: Early Stage Bladder Cancer Prognosis
Treatment Of Irritable Bladder
There is no blanket treatment for irritable bladder syndrome. It largely depends on the underlying cause. The following are standards treatments applied today.
- Antibiotics: Usually prescribed for irritable bladder due to infection
- Bladder training: A technique that teaches the bladder to gain control and improve voiding times. It begins with the patient literally scheduling a bathroom visit even if he or she does not feel like there is a need to go at that specific time. The interval between bathroom visits is gradually increased towards a goal of about four hours. This idea is that the body adapts to these times and incontinence is eliminated.
- Antispasmodics: Drugs that relax the bladder muscles and can help prevent uncontrolled bladder contractions.
It is important to know that pads and diapers are widely marketed today, but many doctors dont recommend them for long-term use. They like to see their patients try to address the problem head-on with some of the approaches listed above or even with home remedies.
Also Check: How Does Overactive Bladder Medication Work
Weeks Pregnant Lower Back Pain
Does Prolapsed Bladder Cause Low Back An Pain In Stomach Low Back Pain And Nausea Raiditing Into Hip Lower Back Pain When Lying On Floor, Passive Pt In Acute Lower Back Pain Causes Of Pain In Right Side Middle Back Acute Lower Back Pain Right Side Popping Feeling.
Pain From Neck Went Down Into Middle Back Sharp Pain In Lower Back When Stretching Backwards. How To Get To Get Medical Marijuana For Chronic Back Pain Lower Back Pain Deep Squat Throbbing Pain Lower Left Back. Shooting Pain In Middle Left Of Back Extreme Left Lower Back Pain.
Read Also: How To Treat Dog Bladder Infection At Home
Posture Lower Back Pain And Pelvic Floor:
In combination with a normally aligned lumbar spine, this arrangement protects the organs of the small pelvis. These normally lie on top of each other and rest on the pelvic floor. If posture is weak, the forces acting on these organs change and complications can occur in the long term. Complications include, for example, a rectocele or cystoycele.
What To Expect At Your Providers Office
When you are seen by a provider, there are several different tests that can help figure out what is going on. These include:
-
Urine tests: These tests can help confirm the presence of blood, as well as check for things like infection.
-
Blood tests: These can include a complete blood count, as well as an electrolyte panel, which tests kidney function.
-
Imaging: Tests like ultrasounds and CT scans can take a closer look at the urinary tract and kidneys. But these are not always necessary to determine the cause of blood in the urine.
In some cases, your provider may suggest you see a medical specialist called a urologist. They can run even more tests if the diagnosis is unclear. This often includes a cystoscopy, which is when they use a tiny camera to look at the bladder.
You May Like: Bladder Leakage Pads For Women
How Is A Cystocele Diagnosed
The doctor may also perform certain tests, including the following:
- Urodynamics: Measures the bladders ability to hold and release urine.
- Cystoscopy : A long tube-like instrument is passed through the urethra to examine the bladder and urinary tract for malformations, blockages, tumors, or stones.
Recovery Time And Instructions Following Surgery
Most women stay in hospital for one, two or three nights.
It is MOST important to rest after the operation and allow the area to heal.
You will be seen by Dr Carey 5 weeks following surgery to check for any problems and remove the S-POP device. You will also have a final review with Dr Carey 12 months following surgery.
Generally it is recommended to..
- Completely restrict your level of physical activity for two weeks.
- From two to four weeks do light activity only.
- Avoid heavy lifting for four weeks, including small children.
- Abstain from sexual intercourse for six weeks.
- Avoid playing sport and impact exercises such as jogging or jumping for four weeks.
Pain relief
- If you experience pain after discharge we suggest that you take pain control medication every four hours as required until pain resolves.
- Make sure you take some time each day to rest.
Maintain good bowel habits
- Try do drink approximately 1.5 litres of fluids each day.
- Maintain a healthy diet.
- Use Movicol or similar preparations if required to maintain regular bowel function and to keep your bowel motions soft.
Any stitches that you still have in when you go home will dissolve in about 10 days . These do not need to be removed.
Dr Carey will be happy to answer any questions you may have and can give more specific advice. Before deciding to have surgery, you should read carefully all the information about your operation and consider obtaining a second opinion.
Recommended Reading: Capsaicin Pills For Overactive Bladder
What Are The Symptoms Of Bladder Prolapse
Sometime bladder prolapse may not cause symptoms. Other times, the symptoms can be bothersome. The most common one is the feeling of heavy pressure in the pelvis and vaginal area. Other signs and symptoms are:
- Frequent urge to urinate
- Involuntary loss of urine
- Still feeling need to urinate after emptying bladder
- Frequent urinary tract infections
Are My Recurrent Urinary Tract Infections Caused By Prolapse
A urinary tract infection is an infection of any part of the urinary tract, including the urethra, bladder, ureters or kidneys. A UTI occurs when bacteria travels into the urethra and up the urinary tract. UTI symptoms may include urinary urgency, frequency, and painful urination. In cases of more severe infections, hematuria , back pain, fever, nausea and vomiting can occur. UTIs may also be asymptomatic , found on urine analysis and culture.
Recurrent UTIs may be related to a variety of sources including kidney stones, fecal incontinence, urinary incontinence, urinary retention, cystocele, rectocele, enterocele or uterine prolapse. In some women, UTIs may occur after intercourse.
A prolapse may cause incomplete bladder emptying allowing for stagnation of urine and bacterial growth. When the cause for recurrent UTIs is prolapse, vaginal prolapse repair or sacrocolpopexy may be suggested to restore the pelvic anatomy, allowing the bladder to empty completely.
In cases of fecal or urinary incontinence, treating the incontinence may help prevent UTIs. Treatments for fecal or urinary incontinence include behavioral changes, medication therapy, pelvic floor physical therapy, mid-urethral sling, InterStim or .
Bladder Pain Syndrome may mimic a UTI but result in negative urine cultures. BPS is not treated with antibiotics.
Recommended Reading: Bladder Stones In Dogs Surgery
What Is A Web Resource Rating
Evaluations that tell you whether free resources on the internet are based on scientific research
- Resource type: Article
Summary – The message of this resource is:
See your doctor if you see blood in your urine. This resource includes questions to ask at your appointment. Blood in urine can be caused by urinary tract infections, kidney stones and bladder cancer and there are effective ways to prevent these conditions.
hematuria, pee, UTI, kidney infection, bladder, prostate, cystoscopy
Browse topics
Is this information reliable, based on scientific research?
Step 2 – Transparency
Is it clear who developed the resource and how?
Step 3 – Usability
Is the information easy to understand and easy to use?
Rated on: 9/13/2016 2:16:24 PM
Related Web Resources
Risk Of Diagnostic Testing
Routine evaluation of all men and women older than 35 years with cystoscopy and CT urography has substantial cost and adverse event implications. In patients undergoing outpatient cystoscopy, 50% reported dysuria and 3% had a documented urinary tract infection 20. In addition, nephropathy from intravenous contrast has been calculated to be greater than 2% in the general population and greater than 2030% in high-risk patients 21. Diagnostic CT scans involve much higher doses of radiation compared with plain-film radiography. It has been estimated that up to 2% of future malignancies may be iatrogenic secondary to CT radiation exposure, and the risk is greater when CT radiation exposure is administered to individuals younger than 40 years 22. The expected detection rate of cancer from a given test should exceed the potential risk of cancer that the test precipitates. Computed tomography scans for women younger than 40 years have the greatest risk and lowest yield in the evaluation of microscopic hematuria.
Don’t Miss: Does Lemon Water Help Bladder Infections
Is The Blood Always Visible
Not everyone diagnosed with bladder cancer has the symptom of blood in the urine that is easily visible, however. Some patients have blood in their urine that is not visible to the eye, because the amount of blood is very small. This symptom is called microscopic hematuria, because the blood is only visible using laboratory tests or a microscope to examine the urine sample. Some patients who are diagnosed with bladder cancer may never notice any symptoms, but their healthcare provider is able to detect the potential presence of blood in their urine during a general check-up, for example. However, this is a less common symptom than visible blood in the urine.
What Does A Prolapsed Bladder Feel Like
A dropped bladder will have different symptoms based on the grade of the prolapse. Many people with a grade 1 prolapse may not experience any symptoms, or they may be very mild.
A prolapsed bladder can also cause you to experience bladder leaks since the bladder and urethra have less support from the pelvic floor muscles. You may also experience pain during sex.
Gravity can play a role in your symptoms as well. Many women find that their symptoms get worse as the day goes on, especially if they are on their feet a lot. Lying down to rest is helpful when symptoms become too much.
If you are premenopausal, or perimenopausal, you may find that your prolapse symptoms feel more intense just before and during your period. If this is the case, try to plan your activities around these days to keep your symptoms at bay.
In addition to the physical symptoms of a prolapsed bladder, many women often feel an extreme emotional burden when they discover they have a prolapse. Its understandable it can be very unsettling to feel something coming out of your body, especially in such a private area.
Women may also feel that the road to recovery, or feeling like themselves again, is a long haul. While treatments such as physical therapy can be very effective, it takes time for the muscles to strengthen and requires dedication on behalf of the patient to do the appropriate exercises. And, surgical treatments can feel scary or intimidating.
Don’t Miss: Can Anxiety Cause Bladder Leakage
How Is Urinary Incontinence Diagnosed
Urinary incontinence is easy to recognize. The primary symptom most people experience is an involuntary release of urine. But the type and cause of the incontinence can be more difficult to determine and may require a variety of exams and tests. Most physicians will use the following:
A bladder diary Your doctor may have you track your fluid intake and output over several days. This may include any episodes of incontinence or urgency issues. To help you measure the amount of urine you pass during an episode of incontinence, you may be asked to use a calibrated container that fits over your toilet to collect the urine.
Urinalysis A urine sample can be checked for infections, traces of blood, or other abnormalities, such as the presence of cancer cells. A urine culture can assess for infection urine cytology looks for cancer cells.
Blood testsBlood tests can look for chemicals and substances that may relate to conditions causing the incontinence.
Pelvic ultrasound In this imaging test, an ultrasound device is used to create an image of the bladder or other parts of the urinary tract to check for problems.
Postvoid residual measurement In this procedure, the patient empties the bladder completely and the physician uses a device to measure how much urine, if any, remains in the bladder. A large amount of residual urine in the bladder suggests overflow incontinence.
UI is usually curable, and if not, then controllable.
Editors Picks
Why Does Bladder Cancer Cause Hematuria
Blood in the urine is a hemorrhaging of the tumor. When the blood vessels of a tumor rupture, that blood ends up in the urine. Early on, cancer blood vessels are delicate. Small tears occur easily. As a tumor grows and invades nearby tissues and blood vessels, this causes bleeding. Whether in small or large amounts, the blood exits through the urine.1,3
Also Check: What Happens To Bladder After Hysterectomy
Greater Risk For Kidney Infections
Most often, a kidney infection develops from an untreated bladder infection. The bacteria invade through the urethra, affect the bladder, and then infection travels up the ureters to the kidneys.
Typically, you would treat the infection before it reaches the kidneys. But sometimes people put off going to the doctor too long. They might try to treat the bladder infection at home or simply dont notice infection symptoms.
But dehydration makes it more likely that the infection will spread through your urinary tract to your kidneys. See your doctor if you have symptoms of a urinary tract infection, and remember its one of the common effects of dehydration.
Risk Factors For Urinary Incontinence

Other conditions that can lead to incontinence in both males and females are:
- Other medical conditions, such as diabetes
- Neurological condition such as MS, spinal cord injuries, or Parkinsons disease
- Being overweight
- Obstructions along the urinary tract that block the flow of urine
- Certain medications
Recommended Reading: Replacement Air Bladder For Sleep Number Bed
What Causes A Prolapsed Bladder
Factors commonly associated with causing a prolapsed bladder are those that weaken the pelvic floor muscles and ligaments that support the bladder, urethra, uterus, and rectum, which can lead to detachment from the ligaments or pelvic bone where the muscles attach:
- Pregnancy and childbirth is the most common cause of a prolapsed bladder. The delivery process is stressful on the vaginal tissues and muscles, which support a woman’s bladder.
- Aging can lead to the weakening of the muscles.
- Previous pelvic surgery: such as hysterectomy
- Other risk factors that increase the pressure within the abdomen, leading to increased pressure on the pelvic floor muscles include chronic obstructive pulmonary disease , obesity, constipation, and heavy manual labor .