Local Estrogen In The Treatment Of Vvs
In postmenopausal women with vaginal dryness, itching, pain or burning, meta-analyses of randomized controlled trials concluded that vaginal estrogen cream use reduced symptoms in the majority of women, but only few women used them beyond 6 months . A systematic review, published in 2014, concluded that all commercially available vaginal estrogens effectively relieve common vulvovaginal atrophy-related complaints and have additional utility in patients with urinary urgency, frequency or nocturia, stress urinary incontinence and UUI, and recurrent UTIs . However, a recent large RCT concluded that neither the vaginal estradiol tablet nor the over-the-counter vaginal moisturizer provided additional benefit over placebo in reducing postmenopausal VVS .
Recommended Reading: Blue Cross Blue Shield Testosterone Coverage
What Follow Up Is Required In Women Who Have Pessary To Treat Pelvic Organ Prolapse
All women with a long term pessary require regular follow up to ensure that they are not developing complications or problems related to the pessary. Regular checks are performed by a doctor every 4 to 6 months with removal and cleaning of the pessary and inspection of the vaginal tissues before the pessary is replaced. The interval between pessary checks can be extended by the doctor depending on the individual patient and the healthiness of the tissues at the time of the pessary check up.
Immunohistochemistry For Hormone Receptor
Tissues were paraffin-embedded and subjected to immunohistochemical staining. The sections were deparaffinized and rehydrated by rinsing in purified water and treated with 3% H2O2 for 15 min at room temperature. After rinsing three times with purified water, they were heated in an autoclave for 1 h with 10 mM citrate buffer and then incubated with primary antibodies. The estrogen receptor â , estrogen receptor â , progesterone receptor , and androgen receptor antibodies were diluted to a concentration of 1:50. After the appropriate secondary IgG antibody was applied, the sections were incubated with DAB and counterstained with haematoxylin . Finally, the sections were dehydrated in a graded series of ethanol, cleared with xylene, mounted in HISTOMOUNT , and evaluated by light microscopy after receiving cover slips. The proportion of stained cells and the extent of the staining were used as immunoreactive score scale for evaluation by a blinded, independent pathologist. The percentage of positive cells was assigned a score from 0 , 1 , 2 , 3 , or 4 .
Read Also: How Do You Fix Nerve Damage In The Bladder
How Can I Treat Bladder Weakness
There are lots of medications that are available on prescription that are used to treated urinary incontinence. You will need to see your GP to discuss your symptoms so they can decide on the best method of treatment for you. Depending on your type of incontinence will depend on your treatment. Below are links to some of the treatment options available
Some of these treatments will need time to start working so if you need something more immediate to help you feel more comfortable then there are a wide range of feminine continence products available on the market now. Many of these have now been designed to be more discreet and can help to take away the embarrassment of urinary incontinence. You can find more information on the products available here.
Read Also: Can You Take Unisom With Melatonin
Local Oestrogen For Pelvic Floor Disorders: A Systematic Review
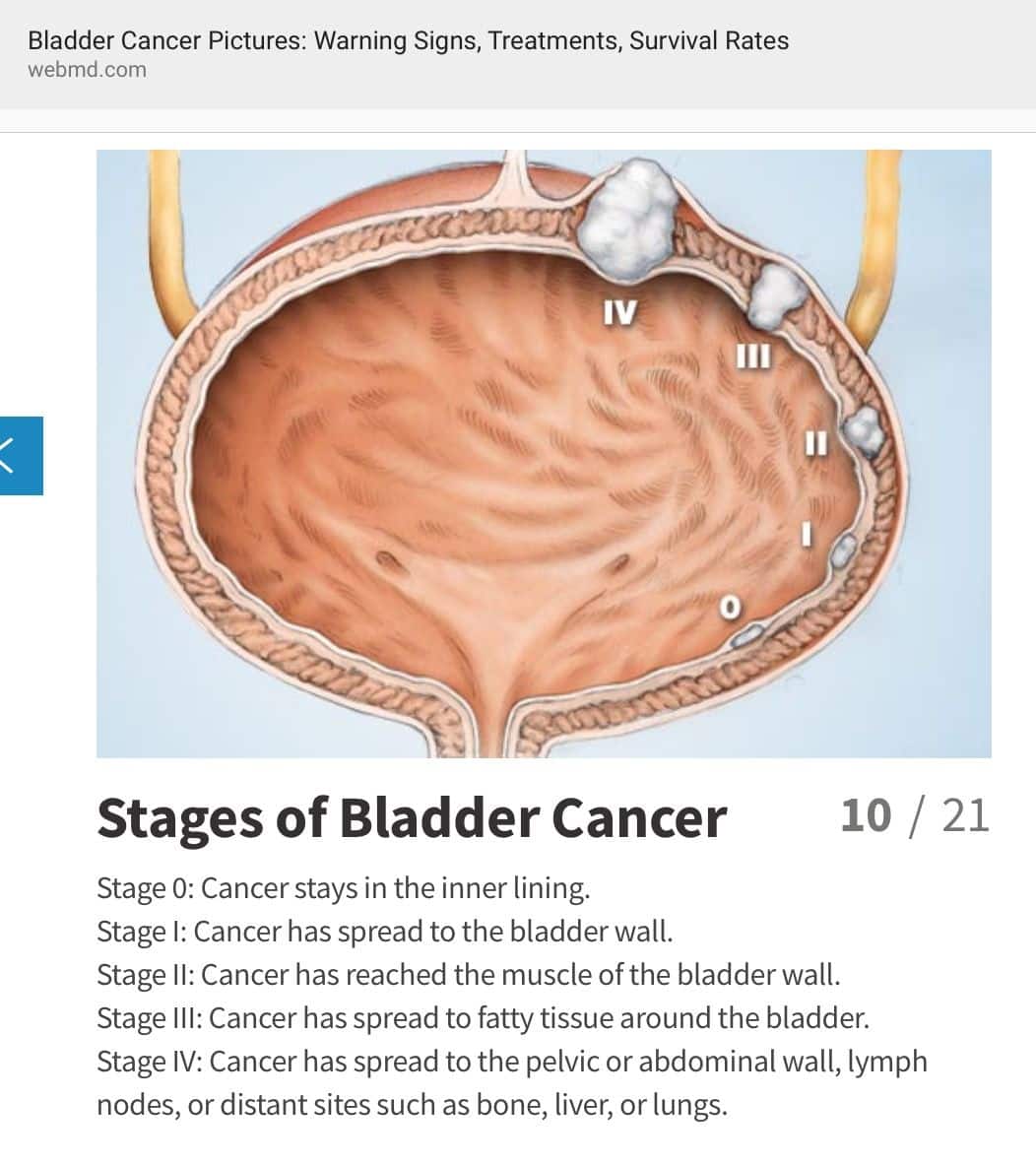
-
Affiliation Department of Obstetrics and Gynaecology, Academic Medical Center, Amsterdam, the Netherlands
-
Affiliation Department of Obstetrics and Gynaecology, Academic Medical Center, Amsterdam, the Netherlands
-
Affiliation Department of Clinical Epidemiology, Biostatistics and Bioinformatics, Academic Medical Center, Amsterdam, the Netherlands
-
Affiliation Medical Library, Academic Medical Center, Amsterdam, the Netherlands
-
Affiliation Department of Obstetrics and Gynaecology, Academic Medical Center, Amsterdam, the Netherlands
-
Affiliation Department of Obstetrics and Gynaecology, Academic Medical Center, Amsterdam, the Netherlands
Read Also: Urge To Urinate When Bladder Is Empty
Could Local Estrogen Therapy Impact The Sexual Function Of Women With Pelvic Organ Prolapse
With regard to sexual function, women with POP may feel self-conscious about their genitals and/or experience pain during sexual intercourse. Additionally, POP can sometimes dampen genital sensations, making stimulation less pleasurable than it was before. All of these factors may result in women with POP avoiding or limiting sexual activity with their partners.
Since sexuality is an important component of many peoples quality of life, treatment options for improving sexual function and sexual satisfaction are often being explored. Many studies have shown that local estrogen therapy can have a positive effect on the sexual functioning of postmenopausal women.
A total of 120 postmenopausal women with POP participated in the study. The women were randomly assigned to the local estrogen cream group or the placebo cream group . Each group was instructed to insert their respective creams with an applicator into their vaginas once a day for one week, every other day for one week, and twice a week for four weeks. .
The researchers used the sexual function domain of the German version of the Pelvic Floor Questionnaire to assess the participants sexual function at baseline and after the six-week treatment period. At the six-week check-in, just over half of the women were sexually active.
At this point, however, women with POP should consider other proven treatment options for their condition such as physical therapy, pessaries , or surgery.
References:
Treatments For Menopausal Pelvic Organ Prolapse
In severe cases, surgical techniques to restructure support for the prolapsed organ are necessary. Usually performed transvaginally, the surgeon will secure the falling vaginal walls, bladder, urethra or other organ in its proper position.
While the use of mesh for pelvic organ prolapse has come under sharp scrutiny in recent years by both the medical community and consumers experiencing long-term side effects, the use of mesh for urinary incontinence is safe and commonly practiced.
Also Check: Can You Have A Bladder Infection Without Uti
Assessment Of Risk Of Bias
Risk of bias was assessed using the Cochrane Risk of Bias Tool . We assessed the risk of bias of the studies that were published after the date of the search in the Cochrane reviews of Suckling , Cody or Ismail or studies that were not included in the Cochrane reviews but were considered relevant for our review. For the studies included in the Cochrane reviews we used the Cochrane authors assessment of risk of bias. Selection, data extraction and risk of bias assessment were performed by two reviewers independently. Disagreements were resolved by discussion, or if necessary, by a third reviewer.
Menopause And Your Urinary Tract
It has been debated whether the changes in a womans urinary tract with age are due to menopause and the lack of estrogen, or instead related to the aging process alone. We do know, however, that the bladder is loaded with estrogen receptors, so the reduction of estrogen that happens in menopause probably doesnt help.
With age, the bladder begins to lose both its volume and its elasticity, and its normal to have to go to the bathroom more frequently. As the bacteria concentration in your genital region increases your urethra may thin, allowing bacteria easier access to your bladder. For these reasons, urinary tract infections are more common as women age. This risk begins to increase within four or five years of your final menstrual period.
The bladder also begins to thin, leaving women more susceptible to incontinence, particularly if certain chronic illnesses or recurrent urinary tract infections are also present.
The pelvic muscles weaken as you age. You may find that exercise, coughing, laughing, lifting heavy objects, or performing any other movement that puts pressure on the bladder can cause small amounts of urine to leak. Lack of regular physical exercise may also contribute to this condition.
Read Also: How Is Botox Administered For Overactive Bladder
Get Effective Treatment With A Team Approach
Women need to know that there are many options available to reduce and sometimes eliminate pelvic organ prolapse. I encourage women not to accept their symptoms as milestones of motherhood or aging. With active research into advanced techniques and new developments each year, women should feel empowered to ask their doctors for the latest treatments for incontinence and pelvic discomfort.
Find out more about pelvic organ prolapse treatment today. Call or request an appointment online.
Influence Of Hrt On Fi
Staller et al. studied the association between HRT and risk of FI among 55.828 postmenopausal women , and current or past use of HRT was associated with a modestly increased risk of FI among postmenopausal women. These results support a potential role for exogenous estrogens in the impairment of the fecal continence mechanism .
Don’t Miss: Yoga Exercises For Bladder Control
Oestrogens And Overactive Bladder
Estrogen has an important role in lower urinary tract function and dysfunction throughout adult life in women. Postmenopausal estrogen deficiency causes atrophic changes in the lower urinary tract and may be associated with urinary frequency, urgency, nocturia, and incontinence. The association of these changes with overactive bladder symptoms is unclear. Systemic and vaginal estrogens have been used for many years during and after menopause to manage urinary dysfunction despite the lack of adequate controlled trials confirming their efficacy. Data from large epidemiological studies have questioned the benefits of systemic estrogens for menopausal symptoms of incontinence and OAB. In the last decade, concerns regarding breast cancer and thromboembolic disease have been led to a marked reduction in the number of women seeking systemic hormone replacement therapy for menopausal symptoms.
The aim of this article was to review current evidence-based data on the effect of exogenous estrogen therapy on lower urinary tract function in menopausal and postmenopausal women, specifically those with symptoms of OAB. Evidence is reviewed on use of both systemic and vaginal estrogen therapy as well as combination therapy with antimuscarinic agents in this population.
Also Check: Can I Take Unisom And Melatonin
Estrogen Affects Your Bladder And Urethra
OAB due to menopause may be an effect of changing estrogen levels. Estrogen is the primary female sex hormone. Your ovaries produce most of your estrogen. Its essential to your sexual health and reproductive system. It also affects the health of other organs and tissues in your body, including your pelvic muscles and urinary tract.
Before menopause, a steady supply of estrogen helps preserve the strength and flexibility of your supportive pelvic and bladder tissues. During perimenopause and menopause, your estrogen levels drop dramatically. This can cause your tissues to weaken. Low estrogen levels may also contribute to muscular pressure around your urethra.
Changes in hormone levels may also increase the risk of urinary tract infections during perimenopause and menopause. UTIs may have similar symptoms as OAB. Talk to your doctor about any new changes to your urinary habits.
Recommended Reading: Galvanized Pressure Tank Vs Bladder Tank
List Of Low Estrogen Bladder Symptoms
Some bladder symptoms that can occur due to low estrogen include:
- Incontinence: This means that a person loses control of their bladder. This can happen in any context. However, one of the most common forms is stress incontinence. This means that a person loses control of the bladder when there is pressure on the pelvic floor, such as when coughing, running, or laughing.
- Urinary pain: A person may have pain when urinating or shortly before or after. Some people notice that their bladder feels painful or full after urinating or that they are unable to fully empty their bladder.
- Overactive bladder : A person may urinate more frequently than usual or have difficulty holding their bladder when they need to use the bathroom.
A person with low estrogen may have genital symptoms, too,
not necessary for a diagnosis. However, doctors may occasionally use:
- vaginal pH testing
- vaginal culture to assess the health of the microbiome
- tissue biopsy, in cases where treatment does not improve the symptoms
If it is unlikely the symptoms are related to menopause, a doctor may perform other tests to rule out other conditions, such as UTIs. They may also assess someones hormone levels, bladder function, or nerve function.
A number of treatments may help with symptoms. They include:
- Hormone replacement therapy : For GSM or vaginal atrophy, a doctor
Some strategies for coping include:
Vaginal Estrogen And Pelvic Floor Physical Therapy In Women With Symptomatic Mild Prolapse
| The safety and scientific validity of this study is the responsibility of the study sponsor and investigators. Listing a study does not mean it has been evaluated by the U.S. Federal Government.Know the risks and potential benefits of clinical studies and talk to your health care provider before participating. Read our disclaimer for details. |
| First Posted : July 24, 2012Last Update Posted : February 4, 2022 |
| Drug: Vaginal estrogenDrug: Placebo | Not Applicable |
- Estrogen therapy in the previous year
- Current or prior breast or pelvic malignancy
- Contraindication to hormone use
Information from the National Library of Medicine
To learn more about this study, you or your doctor may contact the study research staff using the contact information provided by the sponsor.
Please refer to this study by its ClinicalTrials.gov identifier : NCT01648751
Read Also: Urinary Incontinence And Overactive Bladder
We Hope To Change This Story
An ongoing clinical trial is examining the effectiveness of vaginal estrogen a supplemental, nonsurgical therapy to reduce symptom recurrence and spare more women the risks and financial implications of revisional surgeries.
For an appointment, please call Dr. Rahn at to discuss treatments.
Vaginal estrogen, when used prior to surgery, improved the resilience of the connective tissue in the pelvic floor.
David Rahn, M.D.
What Are The Next Steps
No matter the reason, frequent urination doesnt have to take over your life. Answers are only an appointment away.
Because once you know whats causing your frequent urination, youre that much closer to a peaceful nights sleep, uninterrupted jog around the lake or worry-free time doing whatever you like on your own terms.
Donât Miss: Does Nugenix Have An Estrogen Blocker
Recommended Reading: Why Does My Bladder Hurt When I Pee
Vaginal Estrogen Cream: Why And How To Use It
When hormones dont work like theyre supposed to, they can cause a variety of problems. Correcting these hormone levels is tricky and may include treatments that range from dietary changes to surgery. Another potential treatment for hormonal issues is a vaginal estrogen cream. Read on to discover how it works, how to use it, and any side effects you should watch out for.
How To Use Vaginal Estrogen Cream
If youre going through menopause and experiencing some of the discomforts of a hormonal imbalance, estrogen cream can help alleviate some of those symptoms.
To use vaginal estrogen cream, you need to be able to insert it into your vaginal canal. Follow these steps to get your applicator filled with the correct dosage:
- Wash your hands thoroughly with soap and warm water.
- Remove the cap from the tube of vaginal cream.
- Screw the nozzle part of the applicator onto the open end of the tube.
- Find the correct dosage. The applicator has markings on it that indicate how much cream will be inserted. Your doctor will give you the dosage amount they want you to use.
- Gently squeeze the tube so the cream fills the applicator to the required dosage mark.
- Unscrew the applicator from the tube, replace the cap on the tube, and set the tube aside.
How to insert the applicator:
- Lie on your back.
- Pull your knees up toward your chest.
- Press the plunger to release the dosage of estrogen cream.
You need to clean your applicator after each use. Simply pull the plunger to remove it from the applicator barrel. Use mild soap and warm water to clean the applicator barrel and plunger. Dont use hot water or boil the applicator.
Also Check: Stage 3 Bladder Cancer Symptoms
Why Use Vaginal Estrogen Cream
There are many different treatments for symptoms of menopause and low estrogen available today. You could change your diet or lifestyle or even supplement with different products.
Women who are going through menopause experience a dramatic shift in their hormones. As the hormones change and stop monthly periods, they can also create some unpleasant vaginal symptoms, such as:
- Vaginal dryness
- Pain during sex due to lack of natural vaginal lubrication
- Painful urination
- Sudden and frequent need to urinate
Hormones affect vaginal health. During menopause, these same hormones shift, changing vaginal health as well.
Vaginal estrogen cream is used to treat the above-mentioned symptoms, as well as others. It should only be used as prescribed by your doctor. If you have any of the above symptoms and are going through menopause, talk to your doctor. They may want to run a few tests before prescribing a vaginal cream to help alleviate these symptoms.
Estrogen Use Tied To Bladder Control Problems

By Linda Thrasybule, Reuters Health
4 Min Read
NEW YORK – Postmenopausal women who take estrogen for years are more likely to experience incontinence than those on the hormone for a shorter time or not at all, a new study finds.
Of 167 women surveyed in the early 1990s and again in 2004, those who had taken estrogen for five years or more were three to four times more likely to report bladder control problems in the second survey than women who had not taken estrogen or took it for less than five years.
Looking at a patients history of estrogen use may be an important factor in their risk for developing urinary incontinence, said Dr. Gina Northington, an author of the study who specializes in urogynecology at Emory University in Atlanta.
Some women take estrogen after menopause to help with symptoms such as hot flashes and vaginal dryness.
For the study, published in the journal Menopause, 167 postmenopausal women filled out questionnaires in 1993, stating whether they had never used estrogen, used estrogen for less than five years, or used it for five or more years.
Eleven years later, of the 167 women who said they didnt have incontinence problems in the first survey, 47 reported having a new case of urinary incontinence.
And more than 31 of those women said their incontinence made it difficult to perform daily tasks such as shopping, attending social events, visiting friends and exercising.
SOURCE: bit.ly/rRpeug Menopause, October 7, 2011.
Recommended Reading: What Can You Do For A Bladder Infection